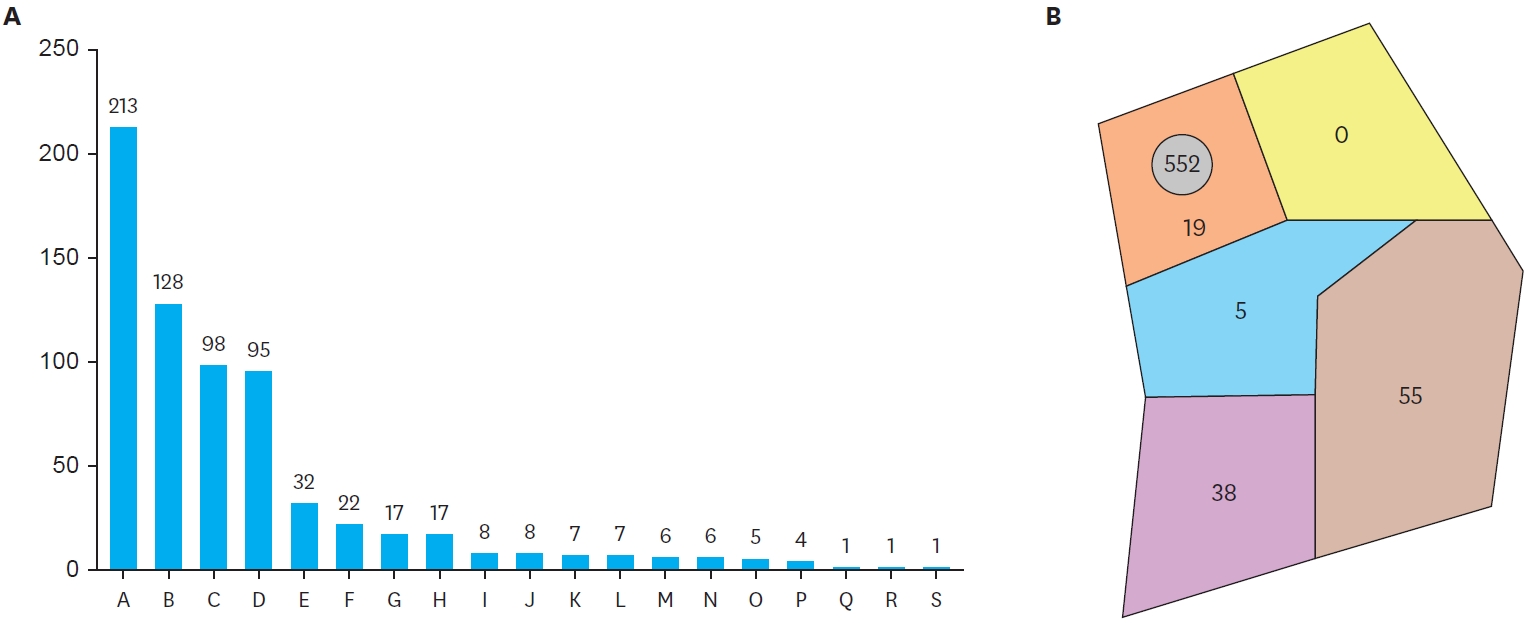
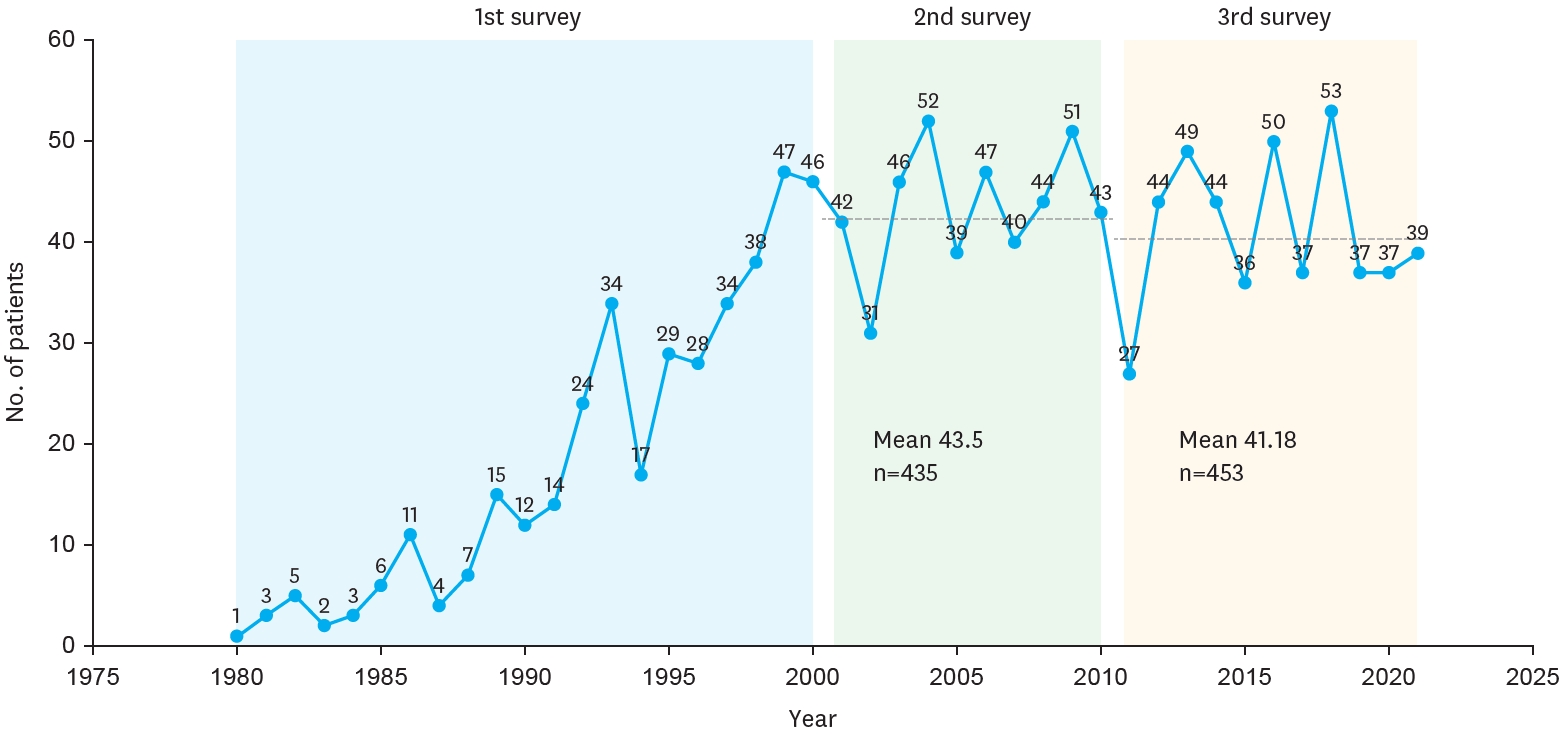
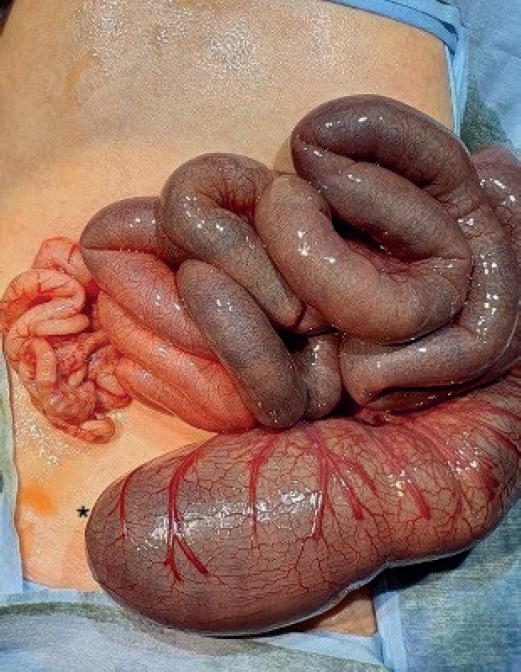
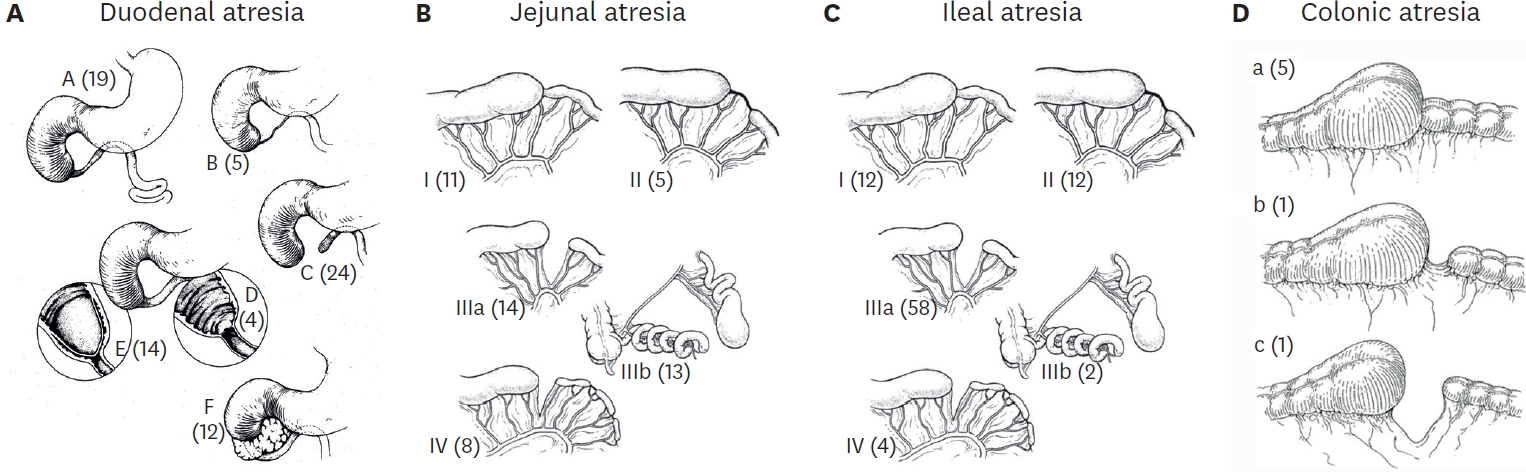
The Korean Association of Pediatric Surgeons (KAPS) performed a nationwide survey on sacrococcygeal teratoma in 2018.
The authors reviewed and analyzed the clinical data of patients who had been treated for sacrococcygeal teratoma by KAPS members from 2008 to 2017.
A total of 189 patients from 18 institutes were registered for the study, which was the first national survey of this disease dealing with a large number of patients in Korea. The results were discussed at the 34th annual meeting of KAPS, which was held in Jeonju on June 21–22, 2018.
We believe that this study could be utilized as a guideline for the treatment of sacrococcygeal teratoma to diminish pediatric surgeons' difficulties in treating this disease and thus lead to better outcomes.
Citations

Although nonoperative treatment of appendicitis (NOTA) in the pediatric population has been well reported recently, patient selection and treatment scheme varies among studies, making it difficult to establish treatment standards for NOTA.
In a single medical center, patients younger than 18 years who were diagnosed with appendicitis: 1) with abdominal pain not exceeding 24 hours, 2) without radiologic evidence of appendicolith or appendiceal perforation or pelvic abscess, and 3) without signs of frank generalized peritonitis were offered NOTA, and their data were prospectively collected.
Twenty-two patients with uncomplicated appendicitis agreed to NOTA and were enrolled in the study. The initial success rate (resolution of abdominal pain and hospital discharge without appendectomy) was 100% (22 out of 22 patients). At a median follow-up period of 23.8 months, two patients had recurrence at two and three months after completion of NOTA. These patients underwent laparoscopic appendectomy.
Stringent patient selection may be necessary to apply NOTA safely for all children with uncomplicated appendicitis. Further studies concerning patient selection and conformed treatment protocols for NOTA are required.
We describe our experience in managing congenital diaphragmatic hernia (CDH) in neonates.
From February 1995 to July 2014, 64 neonates diagnosed with CDH were managed. The medical records of these neonates were retrospectively reviewed.
There were 40 males and 24 females. CDH was on the left side in 44 cases (68.8%), on the right side in 19 cases (29.7%) and bilateral in 1 case (1.6%). Forty-six patients (71.9%) received surgical repair of the hernia while 18 patients (28.1%) died prior to surgery. The timing of surgery was mean 7.0 days after birth. Extracorporeal membrane oxygenation was used in six patients (9.4%), High-frequency oscillation ventilation was used in 49 patients (76.6%), and nitric oxide was used in 42 patients (65.6%). Thirty-three cases (71.7%) of CDH repair were done via open laparotomy, 3 cases (6.6%) by open thoracotomy. and minimally invasive thoracoscopic repair was done in 10 cases (21.7%). Ten cases (21.8%) required patch repair of the CDH. Barotrauma and pneumothorax of the contralateral lung was seen in 16 cases, leading to death in 15 of these cases. The overall survival rate was 48.4% (31/64) and postoperative survival rate was 67.4% (31/46). When all patients are divided into 3 groups by era and analyzed by logistic regression models, the mortality outcome of recent era (2009–2014) was significantly better than that of intermediate era (2002–2008) (29% vs. 71%, p=0.006) and tended to be better than that of past era (1995–2001) (42% vs. 71%, p=0.062).
The overall survival of neonates with CDH at our center has improved over the last two decades. Sixty-four neonates with CDH were managed at a single center and their overall survival was 48.4%. The risk factors for mortality include the occurrence of pneumothorax and right side lesions.
Citations

The congenital H-type rectovestibular fistula, a fistula between the anorectum and genital tract besides a normal anus is a rare variant of anorectal deformities. This disease needs proper treatment but there are no standard of diagnosis and treatment. The purpose of this report is to review a 13-year experience of approach and management for H-type rectovestibular fistula at a single institution.
From February 2002 to August 2015, we cared for 11 patients who had congenital H-type rectovestibular fistula and reviewed their clinical presentation, accompanied anomalies, diagnostic modalities, operative technique, and postoperative progress.
Most patients with H-type rectovestibular fistula presented with symptoms including vestibular defecation and major labial abscess. We could find the fistula tract in most of patients by fistulography using contrast dye. All of the patients had been operated. There were 2 recurrences after surgical treatment who had inflammation and infection associated with the fistula. All other patients recovered without complications.
We think the operation including fistulectomy and repair of perineal body through a transanal approach can be a feasible option to the congenital H-type rectovestibular fistula. Also, combined inflammation and infection should be treated prior to surgery to reduce postoperative complications.
Cervical lymphangiomas are rare lymphovascular malformations arising in the neck, which form huge fluid-containing cysts. Treatment of the malformation consists of surgery and sclerotherapy. However, the optimal approach is still controversial. Here, we describe a series of cervical lymphangiomas which have been treated with surgical approaches.
We retrospectively investigated the medical records of 82 patients who had been diagnosed with cervicofacial lymphangioma from 2001 to 2012 in our center. A closed suction drainage with negative pressure was placed on the operative lesion following excision to prevent reaccumulation of lymphatic fluid and the drainage tube was removed after injecting OK-432 through the tube.
Twelve patients underwent surgical excision of cervical lymphangioma. The median patient age was 3 months at the time of the operation. The patients have been followed-up over a period of 34 months. When lesions were located near vital organs such as the trachea or carotid artery or did not respond to repetitive OK-432 injections, surgical treatment might bring good outcomes. However, swallowing difficulty, lip palsy, or dyslalia due to adjacent nerve damage temporarily appeared as postoperative complications. Five children had tracheostomy due to tracheal or subglottic stenosis and 2 patients had gastrostomy due to aspiration while they eat after surgery.
Surgery for cervicofacial lymphangioma should be conducted carefully in selective cases. A well thought-out surgical plan with a multidisciplinary surgical team approach and placement of closed suction drainage tube after surgery and adjuvant OK-432 sclerotherapy through drainage tube seem to be helpful for good outcome.
Citations

Fundoplication is a common surgical procedure for gastroesophageal reflux Disease (GERD). Recently the procedure has been performed with increased frequency laparoscopically. The aim of this study is to compare laparoscopic Nissen fundoplication (LNF) and open Nissen fundoplication (ONF) for GERD in children. We studied retrospectively the 88 pediatric patients who underwent the Nissen fundoplication for GERD as primary antireflux surgery from 1994 and 2009. ONF was performed in 34 cases and LNF was in 54 cases. 58 patients have neurologic impairment. Time to initial food intake after the surgery were reduced in the LNF group (
Three hundred and twenty-seven patients of 2,046 inguinal hernia cases primarily repaired at Hanyang University Hospital had the history of incarceration or presented as incarcerated inguinal hernia on admission. Incidence of incarceration of all male hernias was 14.2%(234 patients) and 22.7%(93 patients) of all female cases. Incarceration occurred in 17.3% of all right hernia cases and in 13.7% of all left hernia cases.
The incarceration occurred 52.6% of the hernia patients in the first month of life, 27.3% in the first year, 26.7% in the second year and 7.8% after 2 years of age. Strangulated inguinal hernia occurred in 8 patients: five patients had ovaries involved, two patients intestines, and one patient omentum. Emergency operations were performed on 66 patients(20.2%) because incarcerated hernia could not be reduced by taxis. At the time of operation, the hernia sacs were empty in 140 of 327 patients and the remainders contained omentum(50), small intestine (44), appendix and/or cecum(28), sigmoid colon(2), ovary and/or tube(66), and omental cyst(l).
An elective hernia repair should be performed promptly after presentation of the hernia, especially before 2 years of life because of high incidence of incarceration. In this study, of 327 incarcerated hernia, 187 patients(57.2%) did not have prior history of incarceration and incarceration developed more than 7 days after hernia onset in 95.6%. If the hernia repairs had been performed within 7 days after hernia onset, about half of the incarceration might have been prevented.
The clinical experience of 2,340 inguinal hernia hernia repaired by one pediatic surgeon om 2,079 children at Hanyang University Hospital from September 1979 to December 1993 was analyzed. Of 2,046 patients who had primary hernia repairs at Hanyang University Hospital, 1,636 were male and 410 female, and 55.5% of hernias occurred on the right side, 36.0 % on the left, and 8.6% were bilateral. The patients presented hernia under the age of 12 months were 45.3% and those performed herniotomy under the age of 12 months were 25.5%. Birth weight was less than 2.5kg in III patients(8.7%) of 1,279 data available patients. Ninety(6.6%) of 1,354 data available patients were premature (<37wks gestation). The proportions of bilateral inguinal hernia and the onset age under 12 months of life in low birth weight babies and premature babies were higher than in full - term babies. Incarcerated inguinal hernia occurred in 327 patients(16.0%) of whom 8 patients were strangulated hernias. The occurrence of incarceration inversely related with age of patients. The subsequent contralateral inguinal l1ernia following unilateral hernia repairs occurred in 80 patients(4.3%) among which 72 were male and 8 were female. The incidence of contralateral inguinal hernia was more frequent in boys(4.8%) than girls (2.2%) and in cases after left herniotomy(6.4%) than after right herniotomy(2.9%). Sixty percent of contralateral inguinal hernia developed within 1 year after primary hernia repair. The recurrence of inguinal hernia occurred in 6 patients(0.27%) treated at our hospital primarily. There were one or more associated congenital anomalies in 83 patients of which congenital heart diseases were the most common. Sliding hernia occurred in 25 patients consisted of 5 boys and 20 girls. Family history was noted in 35 patients and there were 28 sets of monozygotic and 3 sets of dizygotic twins.

