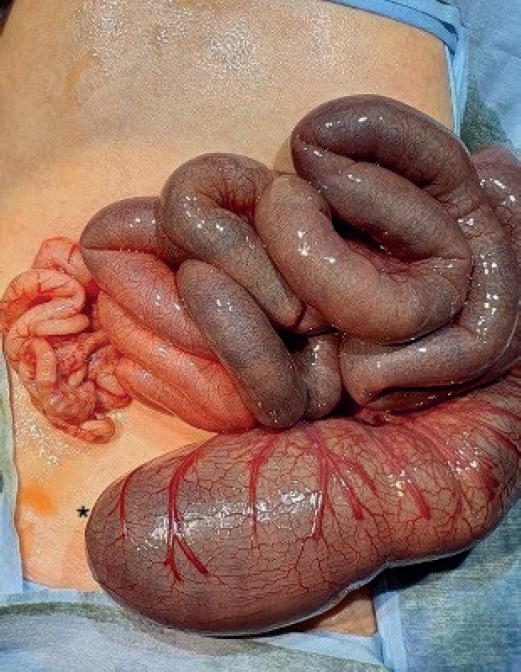
Total proctocolectomy with ileal pouch-anal anastomosis (T-IPAA) in childhood is a surgical procedure mainly applied to familial adenomatous polyposis (FAP) or ulcerative colitis (UC), but it can be applied to non-FAP/non-UC disease (NFNU). Studies regarding the role of T-IPAA who underwent the operation in childhood, especially in terms of long-term gastrointestinal function, complications, and quality of life (QOL) are limited. The aim of this study was to evaluate the characteristics of patients receiving T-IPAA and to compare their bowel function outcomes and QOL.
Patients aged ≤18 years at the time of T-IPAA were included. Their medical records were retrospectively reviewed. Krickenbeck classification, Cleveland Clinic Incontinence (CCI) score, 36-item Short-form Health Survey Questionnaire, and Gastrointestinal Quality of Life Index were used for the evaluation of bowel function and QOL. The median follow-up period was 9.8 years.
Of the 25 patients, 9 had FAP, 9 had UC, and 7 had NFNU. NFNU include 3 of Hirschsprung disease, 2 of intestinal neuronal dysplasia, and 2 of imperforate anus. The median age at T-IPAA was 17.8, 14.2, and 9.3 years for FAP, UC, and NFNU, respectively (p=0.001). Bowel function was satisfactory in terms of voluntary bowel movement (VBM), soiling, and constipation. VBM and constipation were not different between the groups, but soiling was most in NFNU (100%, p=0.047). However, QOL was best in the NFNU group in surveys (p=0.034 and 0.004, respectively).
T-IPAA could be safely applied not only for FAP and UC but also for other diseases in selective cases, with caution.
Citations

Barium enema is one of the diagnostic modalities for Hirschsprung'sdisease. The present study aimed to investigate the diagnostic accuracy of barium enema for Hirschsprung's disease, especially total colonic aganglionosis (TCA).
We retrospectively reviewed the medical records of all the patients who were diagnosed as having TCA and underwent a barium enema in Asan Medical Center Children's Hospital between January 1998 and December 2016. All the tests were performed and reviewed by pediatric radiologists.
Among the total 19 patients with TCA who underwent barium enema, 9 patients (47.4%) had accurate radiographic results. Eight of the 13 neonate patients (61.5%) showed typical TCA radiological findings. However, only one of the 6 patients aged >4 weeks (16.7%) had accurate radiological diagnosis.
Barium enema showed low accuracy for TCA, and its diagnostic performance was better in neonatal period than in those aged >4 weeks.
The single stage transanal pull-through (SSPT) for Hirschsprung’s disease is becoming the most popular procedure. This single center study compared the result of single stage operation with two-stage operation for Hirschsprung’s disease in neonates.
We retrospectively reviewed medical records of all patients who were diagnosed as Hirschsprung’s disease and underwent SSPT or two-stage operation operation in Asan Medical Center between January 2003 and July 2014.
There were 17 SSPT and 28 two-stage operation. The mean age of SSPT group was 14.2±7.1 days, and the mean age of two-stage operation group was 15.4±8.6 days for stomy formation, and 188.6±36.3 days for Duhamel operation. The operation time of SSPT was shorter than Duhamel operation (145.0±37.0 minutes vs. 193.0±36.0 minutes, p<0.001). The mean follow-up period of SSPT and two-stage operation was 35.5±34.9 months (range, 2-132 months) and 56.6±35.5 months (range, 1-121 months), respectively. Defecation problem rate such as fecal soiling or fecal impaction showed no significant difference between the two groups (p=0.719). Two SSPT patients required botulinum toxin injection due to rectal stenosis. Three patients of SSPT group underwent re-do endorectal pull-through due to remnant aganglionic or hypoganglionic bowel.
The SSPT showed shorter hospital days. However, few patients experienced rectal stenosis, but were manageable with botulinum toxin injection. The SSPT requires experienced-pathologist, as well as surgeon, because intra-operation pathology reading is critical for appropriate SSPT. SSPT is a feasible and reasonable option to treat Hirschsprung’s disease.
Citations

Hirschsprung’s disease (HD) is a congenital intestinal disorder with absence of ganglion cells in the intestinal muscle and submucosa. Diagnosis is based on histopathological study such as H&E, and acetylcholinesterase (AchE) immunohistochemistry. Calretinin immunohistochemistry was introduced as a new diagnostic method against limitations of other staining. The aim of this study is to investigate the usefulness of calretinin immunohistochemistry for the diagnosis of HD compared to H&E and AchE.
Ten patients with HD and 22 non-HD patients were included in the study. H&E staining, AchE and calretinin immunohistochemistry were performed in all 32 patients. All slides were evaluated by same single pathologist and the diagnostic value was calculated for each H&E stain, AchE immunohistochemical staining, and calretinin immunohistochemical staining.
Calretinin method had sensitivity of 100% and specificity of 100% for diagnosis of HD. Its diagnostic accuracy was 100%. AchE staining showed 100% of specificity and 80% of sensitivity. Diagnostic accuracy of H&E staining was 56.3%.
We concluded that calretinin immunohistochemistry is a very useful and valuable method to diagnosis HD patient.
The purpose of this study was to compare the diagnostic accuracy of the non-invasive diagnostic methods and rectal suction biopsy for the detection of Hirschsprung disease (HD).
We reviewed diagnostic methods and results retrospectively in patients who underwent anorectal manometry, barium enema and rectal suction biopsy for the diagnosis of HD at Asan Medical Center from January 2000 to December 2012.
There were 97 patients (59 neonates and 38 infants) in the study period. The overall accuracy of anorectal manometry for the diagnosis of HD was 71.1% and its sensitivity was 51.4% (48.1% in neonate and 62.5% in infant, respectively) and its overall specificity was 82.3% (81.3% in neonate and 83.3% in infant, respectively). The Overall accuracy of barium enema was 66.0% (72.8% in neonate and 55.3% in infant, respectively) and specificity of barium enema was 53.2% (56.3% in neonate and 50.0% in infant, respectively). These results were lower than those of anorectal manometry. The overall sensitivity of barium enema was 88.6% (92.6% in neonate and 75.0% in infant, respectively) and it was higher than the sensitivity of anorectal manometry. Histological studies confirmed HD in 35 patients, in one of whom the suction biopsy showed negative finding.
Accuracy of non-invasive methods for diagnosis of HD in our study is lower than those in previous study, so we need to improve the quality of diagnostic tools in our hospital. We conclude that the rectal suction biopsy is the most accurate test for diagnosing HD, so the biopsy to confirm the diagnosis of the HD is very important.
Citations


