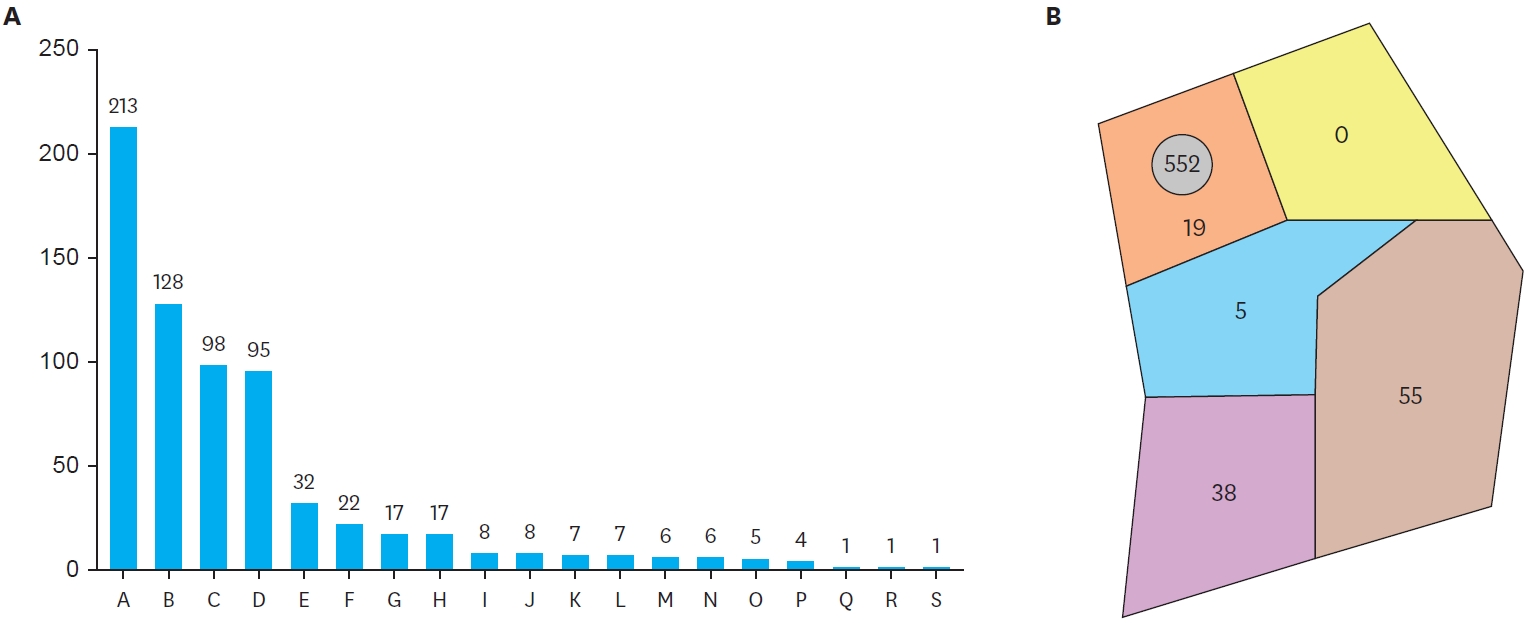
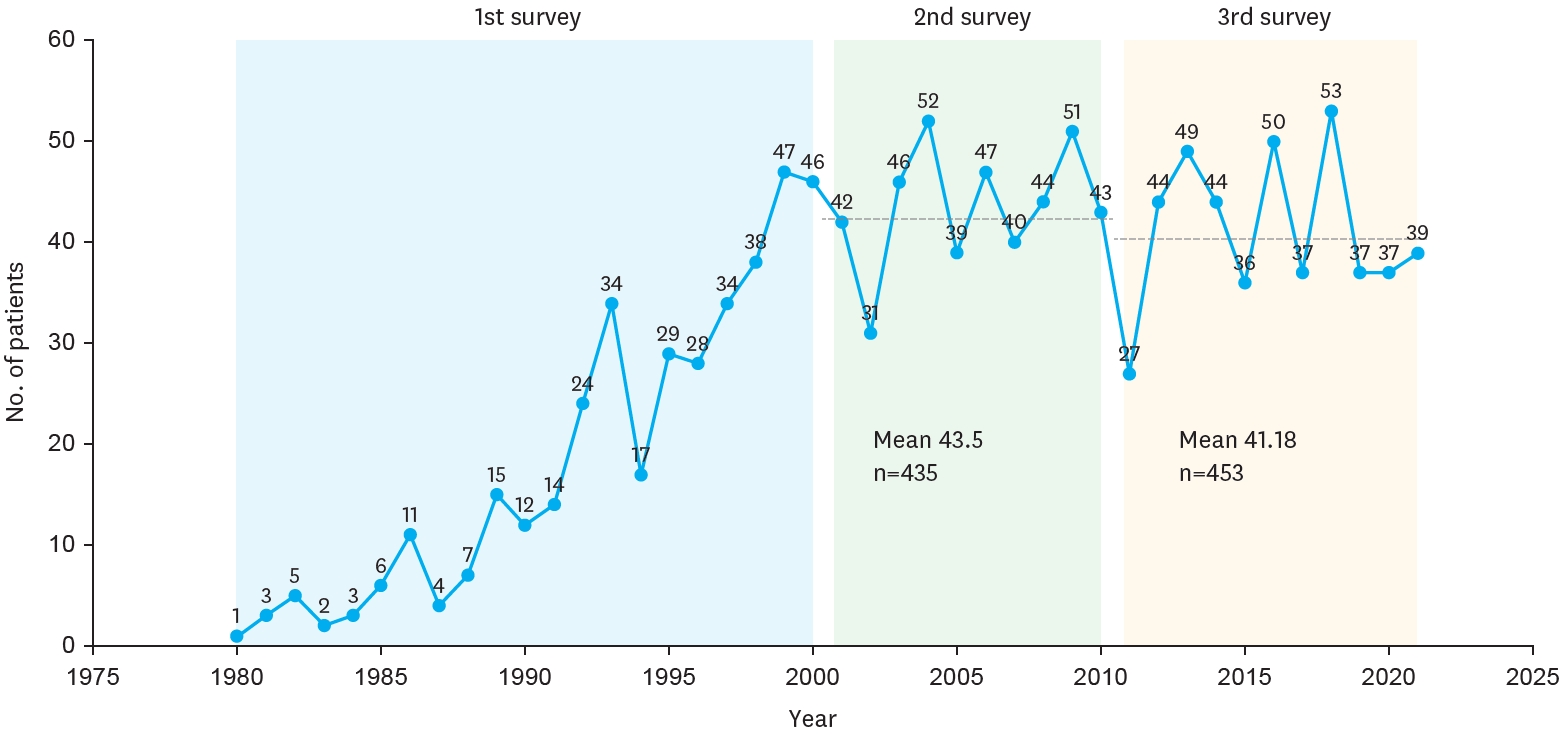
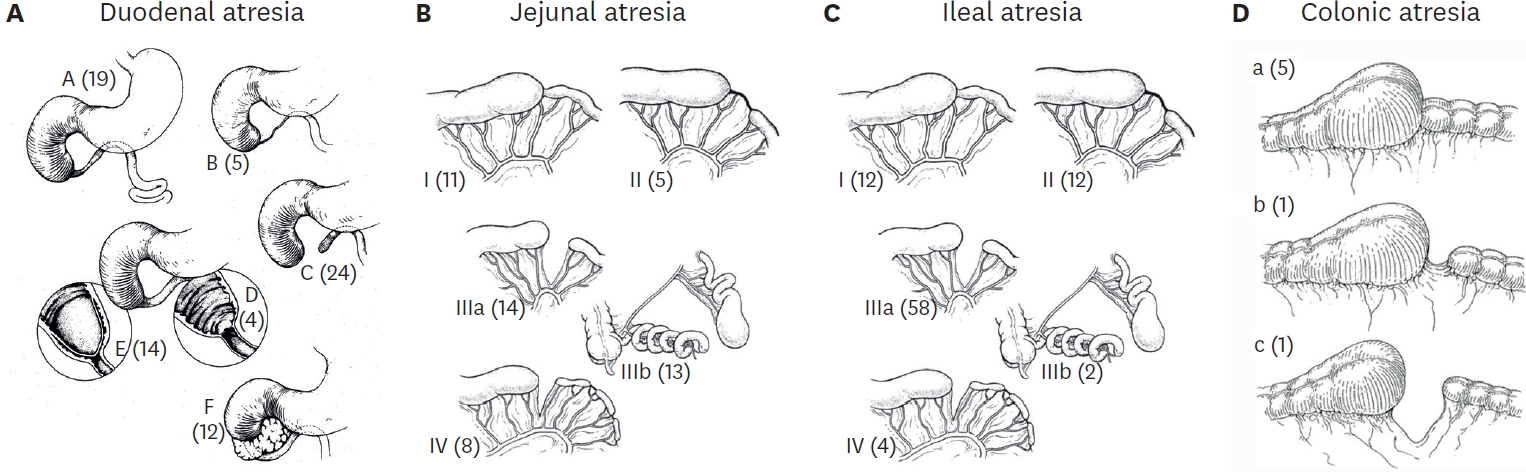
The Korean Association of Pediatric Surgeons (KAPS) performed a nationwide survey on sacrococcygeal teratoma in 2018.
The authors reviewed and analyzed the clinical data of patients who had been treated for sacrococcygeal teratoma by KAPS members from 2008 to 2017.
A total of 189 patients from 18 institutes were registered for the study, which was the first national survey of this disease dealing with a large number of patients in Korea. The results were discussed at the 34th annual meeting of KAPS, which was held in Jeonju on June 21–22, 2018.
We believe that this study could be utilized as a guideline for the treatment of sacrococcygeal teratoma to diminish pediatric surgeons' difficulties in treating this disease and thus lead to better outcomes.
Citations

Lymphatic malformations (LMs) are congenital malformations of the lymphatic system which can be effectively treated by sclerotherapy. This study aims to evaluate the efficacy of doxycycline in the treatment of LMs.
We retrospectively reviewed the medical records of all patients who were diagnosed as LMs and underwent doxycycline sclerotherapy in Asan Medical Center between March 2013 and February 2014. Thirty-five sclerotherapy procedures were performed on 21 patients. The procedures were performed under general anesthesia. After each treatment, the clinical and radiographic response was characterized as complete (≥80% decrease in lesion size), partial (<80% decrease of size), or no response (no decrease of size).
There were 11 male patients and 10 female patients. The median age of sclerotherapy was 21 months (range, 2–180 months). The most common location was cervicofacial (52.3%), followed by extremity (28.6%) and truncal (19.0%). The most common lesion type was macrocystic (71.4%), followed by microcystic (28.5%). There was one (2.8%) skin necrosis which was recovered by wound management. Thirty-eight percent of patients had a complete response, 47.6% of patients had a partial response and 14.3% of patients had no response. Median frequency of treatment was one (range, 1–5). No response group consisted of all microcystic type.
Sclerotherapy with Doxycycline is safe and effective for macrocystic LMs.
Citations

We evaluated perioperative and long-term outcomes of minimally invasive surgery (MIS) and established indications of MIS in solid pseudopapillary tumor (SPT) in pediatric patients.
From October 1992 to April 2018, 66 patients (age, <18 years) diagnosed with SPT underwent either open pancreatectomy (OP) or MIS. Variables including postoperative complications and recurrence rates were retrospectively analyzed.
Thirty-five patients underwent open surgery and 31 underwent laparoscopic/robotic surgery. Mean tumor size in MIS was significantly smaller than that in OP (4.3±1.8 cm vs. 7.6±3.5 cm, p=0.005). There were 4 cases of open conversion from laparoscopic surgery because of vessel encasements (n=2), bleeding (n=1), and pancreatic ductal injury (n=1). Solitary pseudopapillary carcinoma was diagnosed in 6 patients. Recurrence was observed in 3 and 1 patients who underwent OP and MIS, respectively (p=0.634). Tumor size, mass size/abdominal diameter (MS/AD) ratio, and degree of the portal or superior mesenteric vein involvement were the most important indications for MIS.
MIS is being widely used in pediatric surgeries with increased expertise and safety, especially in pancreatic diseases. Careful patient selection for MIS in regards with parameters such as MS/AD ratio and vessel abutment might be a feasible choice.
Citations

Barium enema is one of the diagnostic modalities for Hirschsprung'sdisease. The present study aimed to investigate the diagnostic accuracy of barium enema for Hirschsprung's disease, especially total colonic aganglionosis (TCA).
We retrospectively reviewed the medical records of all the patients who were diagnosed as having TCA and underwent a barium enema in Asan Medical Center Children's Hospital between January 1998 and December 2016. All the tests were performed and reviewed by pediatric radiologists.
Among the total 19 patients with TCA who underwent barium enema, 9 patients (47.4%) had accurate radiographic results. Eight of the 13 neonate patients (61.5%) showed typical TCA radiological findings. However, only one of the 6 patients aged >4 weeks (16.7%) had accurate radiological diagnosis.
Barium enema showed low accuracy for TCA, and its diagnostic performance was better in neonatal period than in those aged >4 weeks.
Spontaneous neonatal gastric perforation is a rare but fatal disease with unclear etiology. In this study, we reviewed its clinical manifestations, outcomes, and discussed the etiology and prognostic factors.
There were 12 neonates with gastric perforation in our hospital from 1989 to 2015. Their medical records were reviewed retrospectively including birth record, associated disease, site and size of perforation, type of surgical management, clinical outcome. Also, the prognostic factors were analyzed.
The median gestational age and birth weight was 32 weeks (range, 26-43 weeks; preterm birth rate, 66.7%) and 1,883 g (range, 470-4,400 g), respectively. Five patients had associated gastrointestinal anomalies including esophageal atresia and tracheoesophageal fistula (two patients), midgut volvulus, non-rotation and microcolon, and meconium plug syndrome. The median age at surgery was six days after birth (range, 2-13 days), and the median weight at surgery was 1,620 g (range, 510-3,240 g). Upper third part of stomach was the most frequently involved location of perforation. The size of perforation varied from pin point to involving the whole greater curvature. Primary repairs were done in seven cases, and in five cases, resections of necrotic portion were needed. Mortality rate was 33.3% (n=4), morbidity (re-operation) rate was 16.7% (n=2). The causes of death were sepsis (n=3), and heart failure from Ebstein anomaly (n=1). The median hospital stay was 92.5 days (range, 1-176 days). The factors mentioned as prognostic factors in previous studies showed no significant relations to the mortality and morbidity in our study.
There were improvements of outcomes in patients with large size perforation. As previous studies, we assume these improvements were possible due to the improvements of critical care medicine. Given that rare incidence, a multi-center study can help us get a better understanding of this disease, and a better outcome.
Hypertrophic pyloric stenosis (HPS) is known to be one of the most common cause of surgery for infants and pyloromyotomy was considered to the standard treatment. There has been an ongoing debate about whether laparoscopic pyloromyotomy (LP) or open pyloromyotomy (OP) is the best option for treating HPS. The aim of this study is to evaluate safety and effectiveness of LP by comparing the clinical results of both surgical strategies performed by single surgeon.
Between January 2000 and December 2013, 60 patients who underwent pyloromyotomy at Asan Medical Center performed by a surgeon were followed: open-supraumbilical incision (n=36) and LP (n=24). The parameters included sex, age and body weight at operation. Clinical outcomes included operation time, time to full feeding, postoperative hospital stay, and postoperative complications.
There were no significant differences in characteristics, postoperative hospital stay between the two groups. Time to full feeding was shorter in LP (OP 24.5 hours vs. LP 19.8 hours; p=0.063). In contrast, the mean operation time was longer in LP (OP 37.5 minutes vs. LP 43.5 minutes; p=0.072). Complications such as perforation of mucosal layer (OP 1 vs. LP 0) and wound problems (OP 2 vs. LP 0) were found to be not worse in laparoscopic group as compared with open group.
There has no difference both laparoscopic and open-supraumbilical incision in terms of postoperative hospital stay, time to full feeds and frequency of complications.
Citations

Gastroschisis and omphalocele are major anterior abdominal wall defects. The purpose of this study was to analyze the clinical differences and mortalities of gastroschisis and omphalocele in Asan Medical Center.
A retrospective review of the medical records was conducted of 103 cases of gastroschisis and omphalocele from September 1989 to February 2013 in Asan Medical Center in Korea.
There were 43 cases (41.7%) of gastroschisis and 60 cases (58.3%) of omphalocele. There was a female predominance in both gastroschisis (60.5%) and omphalocele (58.3%). The average gestational age at delivery was 36.7±0.4 weeks for both groups. The mean birth weights were 2,381.9±80.6 g for gastroschisis and 2,779.4±82.8 g for omphalocele (p=0.001). Mean maternal ages in the gastroschisis and omphalocele groups were 27.5±0.7 years and 30.5±0.7 years, respectively (p=0.002). Associated malformations were documented in 13 infants (30.2±) with gastroschisis and 46 infants (76.7±) with omphalocele (p<0.001). All of gastroschisis patients except one underwent surgery including 31 primary repairs and 11 staged repairs. Fifty-two infants with omphalocele underwent surgery-primary repair in 41 infants and staged repair in 11 infants. Among 103 cases, 19 cases (18.4%) expired. Mortality rates of gastroschisis and omphalocele were 23.3% (10/43 cases) and 15.0% (9/60 cases), respectively (p=0.287). The main causes of death were abdominal compartment syndrome (6/10 cases) in gastroschisis, respiratory failure (4/9 cases) and discharge against medical advice (4/9 cases) in omphalocele.
Gastroschisisis was associated with younger maternal age and lower birth weight than omphalocele. Associated malformations were more common in omphalocele. The mortality rates did not make a statistical significance. This might be the improvement of treatment of cardiac anomalies, because no patient died from cardiac dysfunction in our study. Furthermore, abdominal compartment syndrome might be the main cause of death in gastroschisis.
Citations

The purpose of this study was to compare the diagnostic accuracy of the non-invasive diagnostic methods and rectal suction biopsy for the detection of Hirschsprung disease (HD).
We reviewed diagnostic methods and results retrospectively in patients who underwent anorectal manometry, barium enema and rectal suction biopsy for the diagnosis of HD at Asan Medical Center from January 2000 to December 2012.
There were 97 patients (59 neonates and 38 infants) in the study period. The overall accuracy of anorectal manometry for the diagnosis of HD was 71.1% and its sensitivity was 51.4% (48.1% in neonate and 62.5% in infant, respectively) and its overall specificity was 82.3% (81.3% in neonate and 83.3% in infant, respectively). The Overall accuracy of barium enema was 66.0% (72.8% in neonate and 55.3% in infant, respectively) and specificity of barium enema was 53.2% (56.3% in neonate and 50.0% in infant, respectively). These results were lower than those of anorectal manometry. The overall sensitivity of barium enema was 88.6% (92.6% in neonate and 75.0% in infant, respectively) and it was higher than the sensitivity of anorectal manometry. Histological studies confirmed HD in 35 patients, in one of whom the suction biopsy showed negative finding.
Accuracy of non-invasive methods for diagnosis of HD in our study is lower than those in previous study, so we need to improve the quality of diagnostic tools in our hospital. We conclude that the rectal suction biopsy is the most accurate test for diagnosing HD, so the biopsy to confirm the diagnosis of the HD is very important.
Citations

Tracheoesophageal fistula without esophageal atresia (H-type TEF) is a congenital anomaly that is characterized by a fistula between the posterior wall of the trachea and the anterior wall of the esophagus, not accompanied by esophageal atresia. The purpose of this study is to investigate the clinical characteristics, diagnostic time, the side of cervical approach and short term result after surgery by searching medical records of patients treated for H-type TEF. The search was done at University of Ulsan, Department of Pediatric Surgery of Asan Medical Center, and the total number of patients from May 1989 to December 2010 was 9 with M:F ratio of 1:2. The median gestational age was 39(+6) (32(+6)~41(+0)) wks. Seven out of nine patients were born at term and the other two were born premature. The clinical presentation was aspiration pneumonia, difficulty in feeding, chronic cough, vomiting, abdominal distension and growth retardation. The symptoms presented right after birth. The diagnosis was made with esophagography and the median time of diagnosis was 52 days of life. The majority of surgical corrections were performed within two weeks of diagnosis (median; 15d, range; 1d - 6m). Six patients had associated anomalies, and cardiac anomalies were most common. The cervical approach was utilized in all cases (right 2, left 7). Transient vocal cord palsy and minor esophageal leakage complicated two cases. Although the diagnosis of H-type TEF was difficult and often delayed, we had a good short term result. The left cervical approach was preferred.
Citations

Extracorporeal membrane oxygenation (ECMO) has been utilized in congenital diaphragmatic hernia (CDH) patients with severe respiratory failure unresponsive to conventional medical treatment. We retrospectively reviewed 12 CDH patients who were treated using ECMO in our center between April 2008 and February 2011. The pre ECMO and on ECMO variables analyzed included gestational age, sex, birth weight, age at the time of ECMO cannulation, arterial blood gas analysis results, CDH location, timing of CDH repair operation, complications and survival. There were 9 boys and 3 girls. All patients were prenatally diagnosed. Mean gestational age was 38.8 ± 1.7 weeks and mean birth weight was 3031 ± 499 gram. Mean age at the time of ECMO cannulation was 29.9 ± 28.9 hours. There were 4 patients who survived. Survivors showed higher 5 min Apgar scores (8.25 ± 0.96 vs. 7.00 ± 1.20,
Citations

Currarino syndrome is a hereditary syndrome characterized by the triad of a sacral bony defect, presacral mass and anorectal malformation. We retrospectively reviewed 13 Currarino syndrome patients who were treated in our center between 1997 and 2010. Demographic data, initial symptoms, initial diagnosis, pathologic diagnosis of presacral mass, associated anomalies and managements were analyzed. There were 8 boys and 5 girls. Four patients were diagnosed as Currarino syndrome immediately after birth with failure of passage of meconium and abdominal distension. Four patients underwent surgery for imperforate anus immediately after birth and were diagnosed as Currarino syndrome later and underwent reoperation. Three patients were diagnosed during work-up and management with of the tentative diagnosis of Hirschsprung's disease. Diagnosis of the remaining two patients was at the age of 26 months and 9 years and anorectal malformation was not associated. Twelve patients showed hemi-sacrum and one patient showed bilateral sacral subtotal agenesis. Two patients without anorectal malformation underwent presacral mass excision, untethering of spinal cord and repair of myelomeningocele. Six out of 8 patients, excluding 3 that expired or were lost to follow up, with anorectal malformation underwent colostomy, presacral mass excision, untethering of spinal cord, repair of myelomeningocele, posterior sagittal anorectoplasty and colostomy repair. One patient underwent only posterior sagittal anorectoplasty after colostomy. One waits the scheduled operation only with Hegar dilatation. Pathologic examation of presacral masses showed myelomeningoceles in 4 patients, lipomyelomeningoceles in 3 patients and dermoid cyst in one patient. Teratoma was combined in 2 patients. Eight patients needed neurosurgical operation for spinal cord problems. Seven patients had urologic anomalies and two of them underwent operation. Currarino syndrome should be considered as a differential diagnosis in pediatric patients with abdominal distension, constipation and anorectal malformation. For proper evaluation and treatment, a multi-disciplinary approach is recommended.
Citations

Meckel's diverticulum (MD) has various clinical presentations and due to the limitation of imaging studies, pre-operative diagnosis is a challenge in pediatric patients. Recently, laparoscopic exploration has been suggested as a favorable method for the diagnosis and treatment of complicated MD. We investigated the results of laparoscopic-assisted surgery compared with open technique. We retrospectively studied patients who underwent resection of complicated MD at our institute from 1997 to 2010 and compared 11 treated by laparoscopic-assisted diverticulectomy (LD) with 11 treated by open diverticulectomy (OD) for complicated MD. Operation time was not significantly different in the two groups. Hospital stay and time to diet were not significantly different. Two patients were re-admitted due to mechanical ileus in the LD group. None of patients in either group needed re-operation. Considering the possibility of false-positive results with imaging studies and the cosmetic benefit, laparoscopic-assisted surgery is a safe and effective treatment modality to diagnose and treat complicated Meckel's diverticulum.
Citations

Pulmonary sequestration (PS) is a rare congenital malformation of the lower respiratory tract. The anomaly is characterized by absence of communication with the tracheobronchial tree and isolated blood supply from an anomalous systemic vessels. With the utilization of antenatal ultrasound, the diagnosis of asymptomatic neonatal PS has increased. Treatment options include observation, arterial embolization and surgical resection. The aim of the present study is to review the clinical course of PS and to share our experience with thoracoscopic resection. A total of 96 patients with PS were treated at Asan Children's Hospital between 1999 and 2010. The diagnosis of PS was established by CT in the cases managed by observation or embolization, and by tissue pathology in the surgical cases. Medical records and radiographic images were retrospectively reviewed. Thirty-nine patients were managed by embolization and 30 patients by surgery. The remaining 27 patients have been under observation without any procedures. Among 27 observation patients, 1 patient regressed completely and 10 patients were lost to follow up. Of the 39 embolizations patients, 2 had their lesion regress and sepsis was suspected after embolization. In 1 patient, the microcoil migrated to the iliac artery during the embolization procedure, and another patient developed renal abscess caused by renal artery embolization. Among 30 surgical cases, resection by thoracotomy was performed in 27 at the Department of Thoracic Surgery, and thoracoscopic resection in 3 at the Division of Pediatric Sugery. Only one wound complication ocurred. We conclud that surgical excision should be recommended for pulmonary sequestration, whether the sequestration is symptomatic or not because of the risk of infection, the low rate of natural regress, poor compliance, severe complications after embolization, and to exclude other pathology. In summary, thoracoscopic resection of the pulmonary sequestration is feasible, efficacious, safe and cosmetically superior even in neonatal period.
Malignant ovarian tumors in children are very rare, and consist of about 1% of all childhood malignant tumors. The purpose of this study is to examine the clinical characteristics, treatment, and prognosis for children with malignant ovarian tumors. We retrospectively reviewed the medical records of children under 15 years of age with malignant ovarian tumors who had been treated surgically at Asan Medical Center between 1989 and March 2009. There were 32 patients, ranged in age at surgery from 2 to 15 years (mean; 10.4 years). The median follow-up period was 64.7 months (from 1 month to 188 months). Pathologic diagnosis were; immature teratoma (n=10), mixed germ cell tumor (n=10), and dysgerminoma (n=6). Tumor stage was classified by the staging system of the International Federation of Gynecology and Obstetrics (FIGO). The number of patients in stage I, II, III, and IV were 24 (75%), 2 (6.2%), 4 (12.5%), and 2 (6.1%), respectively. The tumor recurred in 4 patients. Seven patients of group 1 did not receive postoperative adjuvant chemotherapy, and in three of them, the tumor recurred. Twenty-five patients (group 2) underwent postoperative adjuvant chemotherapy, and there was only one recurrence. One patient who did not receive postoperative adjuvant chemotherapy and expired 10 months after operation because of tumor recurrence and distant metastasis. The overall 5-year event free survival (EFS) was 84.2%: group 1 in 44.4%, and group 2 in 95.7%. Tumor recurrence was related to the postoperative adjuvant chemotherapy (p=0.004). In conclusion, proper surgical procedures with relevant postoperative adjuvant chemotherapy might improve clinical results in children with malignant ovarian tumors.
Hickman catheters are tunneled central venous catheters used for long-term venous access in children with malignancies. The appropriate management for various kinds of catheter related complications has become a major issue. We retrospectively analyzed the clinical, demographic, and surgical characteristics in 154 pediatric hemato-oncology patients who underwent Hickman catheter insertion between January 2005 and December 2009. There were 92 boys and 62 girls. The mean age at surgery was 7.6±5.1 years old. The mean operation time was 67.4±21.3 minutes and C-arm fluoroscopy was used in 47(30.5%). The causes of Hickman catheter removal were termination of use in 82 (57.3%), catheter related bloodstream infection in 44(30.8%), mechanical malfunction in 11(7.7%), and accidents in 6(4.2%). Univariate and multivariate analysis for associated factors with catheter related bloodstream infection showed that there were no statistically significant associated factors with catheter related infection complications. All cases except two showed clinical improvement with catheter removal and relevant antibiotics treatment. The mean catheter maintenance period in patients of catheter removal without complications was 214.9±140.2 days. And, The mean catheter maintenance period in patients of late catheter related bloodstream infection was 198.0±116.0 days. These data suggest that it is important to remove Hickman catheter as soon as possible after the termination of use. When symptoms and signs of complications were noticed, prompt diagnostic approach and management can lead to clinical improvements.
Although the incidence of esophageal atresia (EA) is higher in twins than in singletons by two to three times, EA usually affects only one member of twins. We report one pair of twins concordant for EA. A 31-year-old healthy woman bore monozygotic female twins at 36 weeks of gestation. They weighed 2,216 and 2,480g, respectively. They had EA with distal tracheoesophageal fistula and underwent primary esophageal anastomosis on the birth day and the 2nd day of life, respectively. Twin A also had suspicious antral obstruction and pyloroplasty was done simultaneously with esophageal repair. She needed antral web excision for continued gastric stasis one month after 1st operation and three balloon dilatations of the esophagus. Twin B recovered uneventfully.
Esophageal atresia with double tracheoesophageal fistula is a very rare anomaly and is difficulty to diagnose preoperatively. We treated a full term baby with esophageal atresia with double tracheoesophageal fistula. At the first operation, only the distal tracheoesophageal fistula was identified and ligated. When the upper esophageal pouch was opened, intermittent air leakages in sequence with positive bagging were noticed. However, intraoperative bronchoscopy did not identify a fistula in the proximal pouch, and the operation was completed with end to end anastomosis of the esophagus. On the 7th postoperative day, esophagography showed another tracheoesophageal fistula proximal to the esophageal anastomosis. A wire was placed in the fistula preoperatively under bronchoscopy. At the 2nd operation through the same thoracotomy incision the proximal fistula was identified and ligated. On the 12th postoperative day, esophagography showed neither stricture nor leakage.
Prophylactic contralateral exploration in unilateral inguinal hernia repair is still controversial. The purpose of this study is to analyze the contralateral incidence of hernia and to verify the necessity of the simultaneous contralateral exploration. Infants and children operated on for inguinal hernia or hydrocele at the Department of Pediatric Surgery of Asan Medical Center from January 1996 to December 2005 were analyzed retrospectively. A total of 383 patients (9.8 %) out of 3,925 patients underwent a simultaneous bilateral operation. A total of 222 patients (6.2 %) out of 3,542 patients underwent a secondary metachronous contralateral operation after primary unilateral inguinal hernia or hydrocele repair. Because simultaneous bilateral operation cases included true bilateral inguinal hernia or hydrocele, and unilateral hernia and simultaneous contralateral exploration, bilateral incidence of inguinal hernia and hydrocele could be maximally considered as 15.4% (605 patients). Therefore, the prophylactic contralateral exploration in unilateral inguinal hernia or hydrocele should be determined carefully in considering history and physical examination of the patients, and postoperative complications.
Citations

Recently, the survival rates of extremely low-birth-weight (ELBW) infants have improved with the development of neonatal intensive care. However, these infants were susceptible to intestinal perforation due to prematurity, fluid restriction, and injection of indomethacin, etc. Because of the risks of transportation, anesthesia and surgery itself, peritoneal drainage has been compared with laparotomy. Through our experience, we investigate the usefulness of peritoneal drainage retrospectively. From 1997 to 2007, six ELBW (M:F=5:1) underwent primary peritoneal drainage for intestinal perforation. Their median birth weight was 685 g (405~870) and gestational age was 25+1 weeks (24+3~27+0). We noticed the intestinal perforation at median 10.5 days (8~18) after birth, and placed Penrose drain or Jackson-Pratt drain through right lower quadrant incision under local anesthesia. The cause of intestinal perforation was necrotizing enterocolitis in one patient, but that of the others was not clear. Three patients who showed normal platelet count and stable vital signs recovered uneventfully. Two patients (birth weight less than 500 g) who showed unstable vital signs and low platelet count (12,000 / mm3 to 30,000 / mm3) expired despite aggressive resuscitation. One patient required laparotomy due to persistent intestinal obstruction after drain removal and survived. Our experience shows that peritoneal drainage was an acceptable treatment for ELBW infants and the prognosis was related to vital sign and platelet count at the time of intestinal perforation, and birth weight.
Citations

There is significant morbidity and mortality associated with the combination of esophageal atresia (EA) and duodenal atresia (DA). Nevertheless, the management protocol for the combined anomalies is not well defined. The aim of this study is to review our experience with the combined anomalies of EA and DA. From May 1989 to August 2006, seven neonates were diagnosed as EA with DA at Asan Medical Center. In all cases, the type of EA was proximal EA and distal tracheoesophageal fistula (TEF). The diagnosis of DA was made in theprenatal period in 1, at birth in 4, 4 days after birth in 1 (2 days after EA repair) and at postmortem autopsy in 1. Except the one case where DA was missed initially, primary simultaneous repair was attempted. DA repair with gastrostomy followed by EA repair in 2, EA repair followed by DA repair without gastrostomy in 2, and TEF ligation followed by DA repair with gastrostomy in 1. There were two deaths. One baby had a large posterolateral diaphragmatic hernia, and operative repair was not attempted. The other infant who had a TEF ligation and DA repair with gastrostomy expired from cardiac failure due to a large patent ductus arteriosus. Simultaneous repair of EA and DA appears to be an acceptable management approach for the combined anomalies, but more experience would be required for the selection of the primary repair of both anomalies.
Citations

Lipoblastoma is a rare benign soft tissue tumor occurring in infancy and early childhood. It is characterized by fat lobules with varying degrees of maturity, multivaculoated lipoblasts, fibrocapillary networks and myxoid stroma. Lipoblastoma has a good prognosis with no metastases despite its potential for local invasion. From Jan, 1990 through April, 2007, 12 children underwent the operation for lipoblastoma, 7 boys and 5 girls, diagnosed at median 22 months (5~43 months). Median follow up was 6 year 7 months. Primary sites included back (n=5), intraabdominal (n=2) and one in each of buttock, chest wall, neck, nose and scalp. Tumors presented with a growing mass in 9 patients, abdominal distension in 2, and an incidental finding on chest radiography in one. Complete excisions were done in all patients. There was one recurrence in a patient with a scalp mass. After reoperation, he has been doing well without evidence of recurrence. Lipoblastoma has a favorable prognosis, but recurrence can occur even with complete excision. Regular follow up is necessary to detect recurrences.
Citations

Teratomas arising from totipotential primitive germ cell are composed of 2 or 3 germ cell layers. We reviewed the records of 166 children who underwent the operation for teratoma from Jan, 1990 through April, 2007. There were 40 boys and 126 girls (average age 6.93±5.83 years). Primary sites were ovary (n=88), sacrococcygeum (n=24), testis (n=16), retroperitoneum (n=16), mediastinum (n=8), brain (n=4), thymus (n=3) and a single tumor involved the adrenal gland, neck, middle ear, oropharynx, stomach, pelvis, omentum, chest wall and scalp. Teratomas were mature in 141 patients, and immature in 25. Six patients who had ovarian immature teratomas grade 2 or 3 with peritoneal gliomatosis underwent adjuvant chemotherapy. During follow up period, 6 mature teratomas recurred at sacrococcygeal area (n=1) and contralateral ovary (n=5). Five patients of them underwent reoperation and diagnosed as a mature teratoma, but one who had underwent a left salpingooophrectomy with right ovary cystectomy at initial operation was observed carefully. Teratomas were dominant in female patients and developed at various organs. Complete excision was needed for good prognosis. In case of immature teratoma, complete excision and appropriate chemotherapy according to grading can contribute to favorable results.
Meckel's diverticulum is the most common congenital anomaly of gastrointestinal tract in children. The incidence of complicated Meckel's diverticulum is about 4%. The major complications of Meckel's diverticulum are bleeding, intussusception, obstruction and perforation. The aim of this study was to investigate the clinical manifestations and the role of laparoscopic surgery in complicated Meckel's diverticulum in children. We retrospectively reviewed the medical records of 19 patients with complicated Meckel's diverticulum who underwent operation at Asan Medical Center between Jan. 1990 and Apr. 2007. Male to female ratio was 11:8, and median age was 1 year (1 day-13 years). The most frequent symptom was hematochezia (68%), followed by irritability or abdominal pain (16%), vomiting (11%), and abdominal distension (5%). Two operative procedures were performed; small bowel resection with anastomosis (68%) and diverticulectomy (32%). The operation proven complications of the Meckel's diverticulum were bleeding (68%), intussusception (16%), perforation (11%) and obstruction (5%). Ectopic tissues found by postoperative pathologic examination were gastric (84%) and pancreatic (11%). Hospital stay after laparoscopic operation for bleeding Meckel's was 5 days (median) and average first postoperative feeding was 1.5 days. On the contrary, hospital stay for open surgery was 7 days and first feed was 3 days. In summary, the most common compliation of Meckel's diverticulum in children was bleeding and ectopic gastric tissues were present in 84%. Laparoscopic procedure seemed to be useful for diagnosis as well as for definitive treatment.
Citations

Fundoplication is accepted as an effective treatment of gastroesophageal reflux disease. The recent results of laparoscopic fundoplication demonstrated safety and less morbidity, shorter hospital stay and less pulmonary complication compared to the open operation. Laparoscopic fundoplication has been our first choice of operation for gastroesophageal reflux disease since 2003. Among 29 cases, there were 2 conversion cases because of severe distension of transverse colon and hepatomegaly. We studied 27 consecutive patients operated upon from January 2003 through December 2004. There were 15 boys and 12 girls, ages from 1.5 months to 12 years (median 25.3 months). Body weight ranged from 2.9 kg to 37 kg (median 9.8 kg). Neurological abnormalities were present in 23 patients. Indications for surgery included medically refractory reflux associated with vomiting, pneumopathy, otorhinolaryngologic pathology, failure to thrive, esophagitis, apnea and bradycardia. We used 4-5 trocars of 5 mm or 12 mm with 30° telescope and performed the Nissen technique in all patients. In neurological impaired patients, gastrostomy tube was placed at the time of fundoplication. Median operative time was 130 minutes (70 - 300 minutes). There was no mortality nor intraoperative complication. Twenty-six patients were followed for median of 19 months (8 - 31 months). Four patients (15.4 %), who were all neurological impaired, developed recurrent symptoms of gastroesophageal reflux disease. Two of these patients had reoperation (1 laparoscopic approach, 1 open method). There were significant increases in body weight in 11 patients after fundoplication. Laparoscopic fundoplication is acceptable as a safe and effective method for gastroesophageal reflux disease.
Citations

Chemoport is widely used in pediatric surgery field. But various complications can occur during the process of insertion or removal of chemoport. Surgeons must be familiar with the treatment of these complications. We had one catheter cuts off during chemoport removal, become a catheter embolism. Interventional radiologic removal was successful. Verifying the length of removed catheter and careful observation of the catheter tip during removal procedure is important to prevent the possibility of catheter embolus. Radiologic intervention was accessible to remove the retained catheter.
Laparoscopic cholecystectomy has been increasingly used because of several advantages, less pain, better expectation for cosmesis (requires small incisions), and more rapid recovery compared with open cholecystectomy. Oral intake is tolerated on the day of operation or on the next. In this study, we evaluated the effectiveness and safety of laparoscopic cholecystectomy in children. Nine cases of laparoscopic cholecystectomy for acute and chronic cholecystitis in children were performed at Asan Medical Center between April 2002 and April 2004. Laparoscopic cholecystectomy was performed on a total of 10 patients, but one of them was excluded because of the simultaneous splenectomy for sickle cell anemia. Clinical presentation, operative findings, operation time, length of hospital stay, and postoperative complications were analyzed. Mean age was 10.4 (4–15) years, and only 3 of patients were less than 10 years. One patient was female. In 8 the diagnosis was calculous cholecystitis. Mild adhesions were found in 3 cases and intraoperative bile leakage in 2. There was no conversion to open surgery and there were no vascular, bowel, or bile duct injuries. Mean operation time was 82.2 (20–160) minutes ; mean length of hospital stay was 2.1 (1–3) day. There was no postoperative complication. Laparoscopic cholecystectomy in children was remarkably free of side effects and complications and had a short recovery time. Laparoscopic cholecystectomy for cholecystitis is considered to be a standard procedure in children.
Citations

There are considerable controversies in the management of congenital diaphragmatic hernia. By 1997, early operation, routine chest tube on the ipsilateral side and maintainingrespiratory alkalosis by hyperventilation were our principles (period I). With a transition period from 1998 to 1999, delayed operation with sufficient resuscitation, without routine chest tube, and permissive hypercapnia were adopted as our practice. High frequency oscillatory ventilation (HFOV) and nitric oxide (NO) were applied, if necessary, since year 2000(period II). Sixty-seven cases of neonatal Bochdalek hernia from 1989 to 2005 were reviewed retrospectively. There were 33 and 34 cases in period I and II, respectively. The neonatal survival rates were 60.6 % and 73.5 %, respectively, but the difference was not significant. In period I, prematurity, low birth weight, prenatal diagnosis, inborn, and associated anomalies were considered as the significant poor prognostic factors, all of which were converted to nonsignificant in period II. In summary, improved survival was not observed in later period. The factors considered to be significant for poor prognosis were converted to be nonsignificant after change of the management principle. Therefore, we recommend delayed operation after sufficient period of stabilization and the avoidance of the routine insertion of chest tube. The validity of NO and HFOV needs further investigation.
Citations

VATER association is defined as a combination of 3 or more anomalies-vertebra(V), imperforate anus (A), esophageal atresia with or without tracheoesophageal fistula (TE), renal and radial anomaly(R). We reviewed our experiences in one center to determine etiology, prevalence, clinical manifestation, other associated anomaly and prognosis. Two hundred and twenty-three cases that underwent operations for imperforate anus or esophageal atresia were analyzed retrospectively through medical records at Department of Pediatric Surgery, Asan Medical Center from June, 1989 to July, 2005. The total number of neonates who had been admitted during period of study were 46,773 and VATER association was 9 (0.019 %, 1.92 persons per 10,000 neonates). Median gestational age and birth weight were 37+4wk (35+1 – 41+4) and 2,594 g (1,671–3,660), respectively and median age of mother was 32 years (23–38). There was no family history. Three patients were twins but their counterparts had no anomalies. Patients who have 3 anomalies were 6, 4 anomalies in two and 5 anomalies in one patient. Vertebra anomalies were detected in 7(77.7 %), imperforate anus in 8(88.9 %), esophageal atresia in 5 patients (55.6 %), renal anomaly in 6(66.7 %), and radial anomaly in 5(55.6 %), respectively. Four patients are alive, 2 patients were lost during follow up period. Three patients died due to neonatal sepsis, respiratory dysfunction and cardiac failure. VATER association did not appear to be a definite risk factor, but merely a randomized combination of 5 anomalies. The prognosis was dependent on the other associated anomalies, appropriateness of management and operation. Careful follow-up and aggressive treatmentare required for improving survival and quality of life.
Inguinal hernia is the most common disease treated by the pediatric surgeon. There are several controversial aspects of management 1)the optimal timing of surgical repair, especially for preterm babies, 2)contralateral groin exploration during repair of a clinically unilateral hernia, 3)use of laparoscope in contralateral groin exploration, 4)timing of surgical repair of cord hydrocele, 5)perioperative pain control, 6)perioperative management of anemia. In this survey, we attempted to determine the approach of members of KAPS to these aspects of hernia treatment. A questionnaire by e-mail or FAX was sent to all members. The content of the questionnaire were adapted from the “
Citations

One day surgery in children has been practiced for last 10 years in this institution. This study is to examine its safety and effectiveness for patients younger than 15 years old treated at the Department of Pediatric Surgery, Asan Medical Center, from September. 1996 to December, 2005. A total of 3,709 patients, 37 % of the total pediatric operations, are included in this retrospective study. The most prevalent ages were between 1 and 3 years olds (1,199 patients). Twenty patients were younger than 6 months, and they all had one day surgery safely. Operations were herniorrhaphy in 3,126 patients,followed by excisional biopsy, chemoport removal, and OK 432 injection. There were 12 cases (0.32 %) of unplanned admissions, 7 occurred within 6 months of one day surgery. Perioperative fever was the most common cause of admission in 4 cases. The related conditions of unplanned admission were bleeding in 2 cases and radical surgery in 2. One day surgery in this institution was easily accessible and safe. This is to the result of appropriate selection of patients, cooperation with anesthesiologists, adequate control of postoperative pain, and home care programs.
Major advances in the management of anorectal malformations have been achieved during the last 20 years. Alberto Pena introduced the posterior sagittal anorectoplasty (PSARP) in 1982. He divided all the sphincteric muscles at the exact posterior midline and fully exposed the crucial anatomy. He was able to manage the associated fistula under direct vision with minimal urinary tract injury. The rectum could be placed in the middle of the sphincteric muscle complex. Even with PSARP by Alberto Pena himself, only 37.5% of all cases were considered totally continent. Anorectal malformation is still acontinuing challenge for the pediatric surgeons.
Citations

performed at the time of discharge. There was only one recurrence of adirect inguinal hernia. Necrotizing enterocolitis developed in 17 patients, 11 were operated upon, two had peritoneal drainages, and 9 had enterostomies. Five of 11 surgical infants died after operation and three of the nonsurgical infants died of various complications. Although micropremies have potentially high risks of serious complications and death, the outcome can improve with careful surgical observation and judgment.
Neuroblastoma treatment remains challenging, but has been advanced by the establishment of clinical and biological variables that determine prognostic risks. Initially, stage and age were the prime determinants of survival used in clinical practice. Risk-based therapy currently is the hallmark of neuroblastoma treatment. This study reviewed the results of neuroblastoma in one center. Sixty-three patients with neuroblastoma were treated primarily at our institution from 1989 to 2003. All patients were graded according to the International Neuroblastoma Staging System (INSS) at diagnosis. There were 37 boys and 26 girls. The median age was 2.14 years (range, 33 days-10.2years). The primary site was the adrenal gland in 47, dumbbell shape extended into spinal canal in 6, retroperitoneum in 5, mediastinum in 3, and other sites in 2. The probability of 5-year overall survival (OS) and event free survival (EFS) were 46.7% and 44.2% by Kaplan-Meier method. According to INSS, there were stage 1 in 2, stage 2 in 5, stage 3 in 12, stage 4 in 42, and stage 4s in 2. There were statistically significant differences in the survival rates between patients with stage1, 2 and stage 3, 4(p<0.05). For the stage 3 and 4, the extent of surgical resection determined from the operative records and pathologic reports assessed extent of surgical resection as complete resection, no visible tumor (CR, n=17); minimal residual, visible tumor less than 5% (MR, n=15); partial resection, more residual tumor than MR (PR, n=11). The 5-year OS rate was 57.8, 51.4, and 13.6% for CR, MR, and PR. There is a trend toward higher OS with achieving the completeness of resection (p<0.05). We conclude that age and stage at diagnosis are prognostic factors, and complete excision of the primary tumor can provide better prognosis for patients with stage 3 and 4 neuroblastoma.
Citations

Intestinal obstruction secondary to intraabdominal adhesion is a well-known postoperative complication occurring after appendectomy. The aim of this study was to measure the incidence and clinical manifestations of mechanical intestinal obstruction after appendectomy for perforated appendicitis. We reviewed all of the children (age <16 years) who had been treated for appendicitis at Asan Medical Center between January 1996 and December 2001. Inclusion criterion included either gross or microscopic evidence of appendiceal perforation. Exclusion criteria were interval appendectomy, and patients immune compromised by chemotherapy. Associations of intestinal obstruction with age, sex, operation time, and use of peritoneal drains were analyzed. Four hundred and sixty two open appendectomies for appendicitis were performed at our department. One hundred and seventeen children were treated for perforated appendicitis (78 boys, 39 girls). The mean age was 8.9 years (range 1.5 to 14.8 years). There were no deaths. Eight patients were readmitted due to intestinal obstruction, but there was no readmission due to intestinal obstruction in patients with non-perforated appendicitis. The interval between appendectomy and intestinal obstruction varied from 12 days to 2 year 7 months. Four patients needed laparotomies. In three of four, only adhesiolysis was performed. One child needed small bowel resection combined with adhesiolysis. There was no significant association between age or sex and the development of intestinal obstruction. This was no association with operative time or use of peritoneal drain. Patients who required appendectomy for perforated appendicitis have a higher incidence of postoperative intestinal obstruction than those with nonperforated appendicitis. For the patients with perforated appendicitis, careful operative procedures as well as pre and postoperative managements are required to reduce adhesions and subsequent bowel obstruction.
Citations

The laparoscopic splenectomy (LS) became popular over the last 10 years. The advantage of LS over open splenectomy (OS) includes short hospital stay, improved cosmesis, less development of postoperative intestinal ileus, and less analgesics required. The purpose of this study is to evaluate the outcome of LS at Asan Medical Center from January 1999 to January 2003. The records of 14 consequent children who underwent splenectomy were reviewed retrospectively. Patients characteristics, morbidity, mortality, operative time, blood loss, and hospital stay were analyzed., Seven patients age 5 to 15 years underwent LS under the indications: idiopathic thrombocytic purpura (ITP, n=3), hereditary spherocytosis (n=3), and myelodysplastic syndrome (n=1). Seven patients, age 7 to 16 years, underwent OS during the same period for ITP (n=7). Median operative time was 120 minutes (80 to 170 mins.) in OS, and 270 minutes (110 to 480 mins.) in LS (p<0.05). Median length of hospital stay was 6 days (3 to 8) in OS, and 4 days (3 to 6) in LS (p>0.05). Median splenic length was 12.0 cm (9.2 to 18.0) in OS, 14.0 cm (10.0 to 19.5) (p>0.05). Accessory spleens were identified in 3 of 7 LS and 1 of 7 OS cases. In the LS group, there was no conversion to open surgery. Two patients in LS required blood transfusion postoperatively. LS in children can be performed as effectively and safely as OS.
This study reviews 14 years' experience of esophageal atresia with special emphasis on the clinical profile and the outcome. From May 1989 to February 2003, 65 cases of esophageal atresia (EA) were treated at Asan Medical Center. Boys outnumbered girls 2.4 to 1. Prematutity and low birth weight were 27.7% and 38.5%. Esophageal atresia with distal tracheoesophageal fistula (TEF) was the most common type (87.7%), followed by pure EA and H type fistula. Forty-six patients (70.8%) had one or more associated anomalies, cardiac malformations were the most common. Duodenal atresia was found in 7 cases. There were 6 patients (9.2%) with VATER cluster. VACTERL cluster was present in 18 patients (27.7%), one of who fulfilled the complete syndrome. Waterston group A, B and C made up 21.5%, 40.0% and 38.5% of the total group. Surgical treatment was attempted in 63 patients and deferred in 2 who had severe associated malformations. For EA with distal TEF, primary esophago-esophagostomy was carried out in 51 cases, and division of TEF and gastrostomy in 4 cases and no operation in 2 cases. For pure EA, colonic graft was done in 2 after gastrostomy and esophagostomy, and esophago-esophagostomy was performed in 2 after gastrostomy. Two TEF was carried out in 2 cases with H type TEF. The overall survival rate was 76.9%, and survival by Waterstuon classification was 100% in group A, 80.8% in B and 60.0% in C. Thorough workup for associated anomalies, interdepartmental approach and more careful surgical decision and technique are required to improve the outcome of EA.
Citations

Appendicitis is the most common surgical emergency in childhood. Open techniques have been adopted in children after experiences in various surgical conditions in adults has accumulated. It is debatable whether Laparoscopic appendectomy (LA) is superior to open appendectomy (OA) in children. The goal of this study is to review the results of laparoscopy and laparotomy in the nonperforated appendicitis. The records of 22 patients under 15 years of age who were operated upon for nonperforated appendicitis at Asan Medical Center were analyzed between December 2002 and April 2003. Age, type and length of intervention, frequency of analgesic use, complication, length of hospitalization, and cost for each treatment groups (N=11) were compared. Laparoscopy patients were older (13.0 vs. 10.1 years; p > 0.05), and operative time was longer (55.0 vs. 35.0 minutes; p < 0.05). There was no conversion (OA to LA). The median length of hospital stay was significantly shorter in laparoscopy (3.0 vs. 2.0 days; p < 0.05). The median cost for LA was more expensive (W833, 836 vs. W751,398; p < 0.05). Even though there were higher costs and longer operative times with laparoscopic procedures, the shorter hospital stay was an advantage.
Citations

Necrotizing enterocolitis (NEC) is usually a disease of premature infants, but occasionally it affects the term neonate. Twenty-five infants with NEC were treated at Asan Medical Center between January 2000 and December 2002. and 13 of them were term infants. In each case, the diagnosis of NEC was established by a clinical illness fulfilling the Bell's stage II or III NEC as modified by Walsh or by surgical findings. There were six males and seven females. The birth weight was from 1,960 to 3,700 g. The age at diagnosis was from 1 to 40 days. Four patients had congenital heart disease; one of them had hypothyroidism and cleft palate. Abdominal distension was present in all, and bloody stools in four. One patient had history of hypoglycemia, three had Rota viral infection. Eight patients had leucopoenia (<5.0 × 109/L), Seven had thrombocytopenia (<100 × 109/L), and three severe thrombocytopenia (<50 × 109/L). Laparotomy was required in 10 of the 13 patients. Indications for operation in acute phase were failure to respond to aggressive medical therapy in five, and perforation in three patients. There were two late phase operation for intestinal stricture and fistula. There was no operative complications. Ten of thirteen patients survived (76.9%). Two patients died of septic complication. There was a delayed death due to heart failure. There was a significant difference in survival according to platelet count (50 × 109/L) (p<0.05). Congenital heart disease and Rota viral infection is associated with NEC in term infants and thrombocytopenia and leucopenia in the course may be surgical indications.
Diagnosing Hirschsprung's disease is a clinical challenge. Hirschsprung's disease should be considered in any child who has a history of constipation dating back to the newborn period. We examined diagnostic methods and their results retrospectively in 37 neonates and infants who underwent both barium enema and anorectal manometry for the diagnosis of Hirschsprungs disease at Asan Medical Center between January 1999 and April 2001. Two radiologists and a surgeon repeatedly reviewed both of the diagnostic results. In anorectal manometry, thirty-four studies were in agreement with the definitive diagnosis, giving an overall diagnostic accuracy of 91.9 % (neonate; 100 %, infant; 85.7 %). The accuracy and specificity of barium enema was lower than those of anorectal manometry, but sensitivity was higher. There was no significant difference between the two methods. Both studies showed findings consistent with the final diagnosis. However, discordant results needed further evaluation or close observation to diagnose accurately. We conclude that Hirschsprungs disease should not be diagnosed by only one diagnostic method.
Citations

Gastrointestinal duplications are rare congenital malformation that may require surgical intervention in the neonate, infant, and occasionally the older child. Symptoms produced by duplications vary according to their location, size, type and histology. We report the clinical characteristics and the surgical results of 9 cases of the gastrointestinal duplications treated at at Asan Medical Center between 1989 and 2000. Five patients were boys and four were girls; age of patients ranged from 5 days to 10 years. Eight duplications were cystic and one was tubular. One involved the stomach; five were in the ileum, and two in the cecum. The most common presentation was intestinal obstruction. There was associated anomaly in one patient, pulmonary sequestration and double ureter. Ectopic gastric mucosa was found in two. All patients underwent surgical resection. There was no perioperative mortality or morbidity. Although gastrointestinal duplication is a rare entity, consideration of associated anomalies and being familiar with the anatomy and clinical features are required for adequate management. In cystic form, complete excision is recommended but planned surgery is required for long segment tubular lesion.
Citations

Eleven children with gastroesophageal reflux disease underwent fundoplication. Eight had neurological impairment, two hiatal hernia and one had history of esophageal repair for esophageal atresia. The most common and significant symptom was vomiting (81.8%), followed by recurrent respiratory infections (72.7%) and failure to thrive (72.7%). The most common diagnostic tool was 24 hour esophageal pH study, which showed a pH less than 4 for more than 10% of the total recorded time in 6 among 9 patients. Nissen fundoplication was performed in 10 patients. Thal fundoplication was carried out in one patient with esophageal atresia. Stamm gastrostomy was added for nutritional and/or swallowing problem in all 8 patients with neurological impairment. The median follow up period was 13 months. There were one late death of unrelated cause and one recurrence. The quality of life after antireflux surgery was greatly improved. Antireflux surgery should be done if indicated, and a simultaneous gastrostomy be considered in a patient with neurological impairment.
Henoch-Schonlein purpura is a systemic vasculitis of unknown etiology that is probably related to autoimmune phenomenon. Henoch-Schonlein purpura is characterized by purpuric rash, arthragia, nephritis, and gastrointestinal manifestations. We reviewed 169 children hospitalized with a diagnosis of Henoch-Schonlein purpura at Asan Medical Center between 1989 and 1998. One- hundred thirty-nine (82.2%) had gastrointestinal manifestations including abdominal pain, nausea, vomiting and gastrointestinal bleeding. Surgical consultations were obtained for ten children, and laparotomy was performed on five children. Three children suspected of appendicitis underwent appendectomy. None had the evidence of appendicitis. One child who was suspected of intestinal strangulation revealed, in pathologic review, the hemorrhagic edema of the proximal jejunum and of the distal ileum at laparotomy. Another child underwent resection for hemorrhagic infarct of distal ileum. High suspicion of this disease entity in differential diagnosis of abdominal pain in children can avoid unnecessary laparotomy in most cases. However, the life-threatening gastrointestinal complications may occur in a small percent of cases. The prompt recognition and adequate radiologic evaluation of abdominal manifestation of this entity is needed for an early surgical intervention.
Congenital afibrinogenemia is a rare disorder that refers to a congenital lack of production of fibrinogen, a key component of the hemostatic system. Bleeding manifestations of congenital afibrinogenemia vary in severity from mild to catastrophic. This is a case report of splenic rupture occurred in an eight-year-old boy with congenital afibrinogenemia. Nonoperative treatment with cryoprecipitate and virally inactivated, purified fibrinogen concentrates successfully avoided splenectomy.
Citations

The results of hepatic portojejunostomy in 34 patients with biliary atresia operated upon by one surgeon between May 1989 and December 1997 were analyzed. Eleven (32.3 %) patients were 60 days or younger, 14 patient (41.2 %) were between 60 and 90 days, and 9 (26.5 %) were over 90 days of age. Jaundice cleared in 20 cases (58.8 %). Three patients died of liver insufficiency, 2 were anicteric but died from esophageal variceal bleeding. Three patients died as a result of sepsis, heart failure and left kidney agenesis. Five patients were lost to follow-up. The five-year survival rate was 73.8 %. Two patients over 90 days of age, survived more than 5 years. Survival rates were not significantly related to the age at operation. We conclude that hepatic portojejunostomy should be considered as a primary surgical modality for biliary atresia, even at age 90 days or more. Early detection of esophageal varices and sclerotherapy may be necessary. Liver transplantation is necessary if hepatic failure develops.

