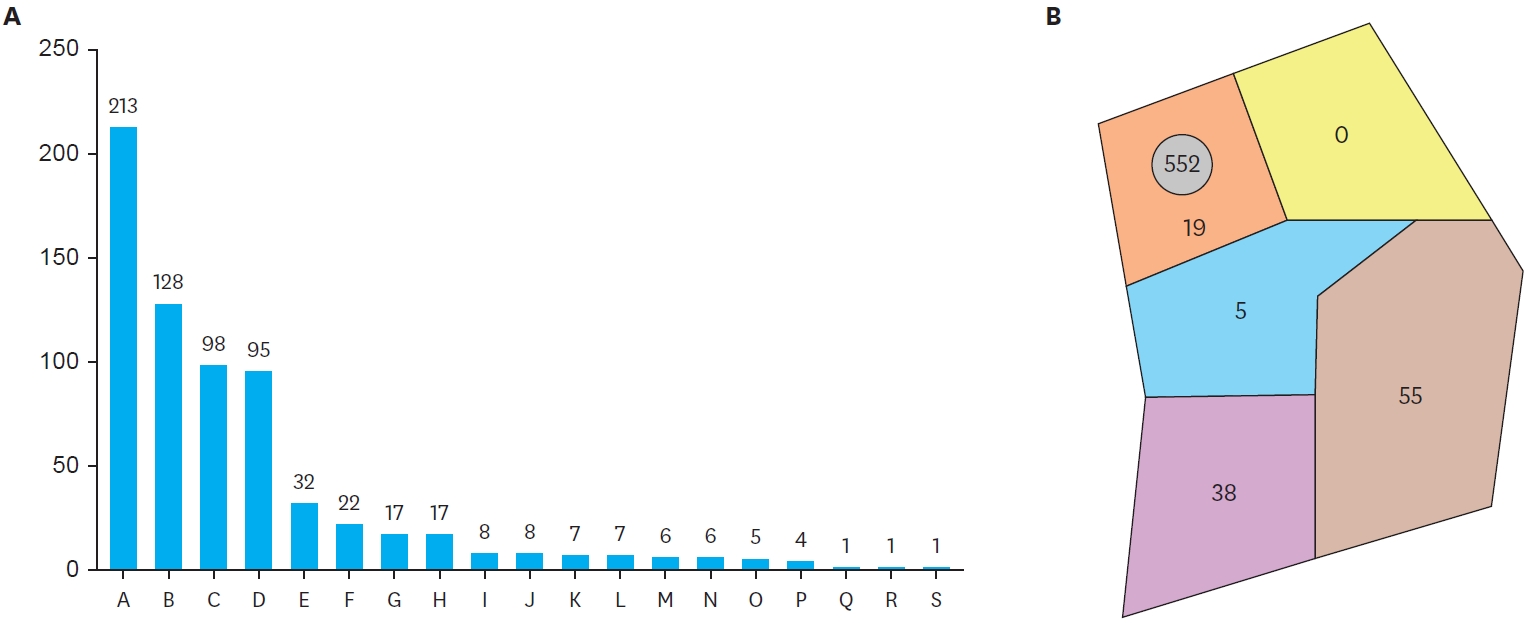
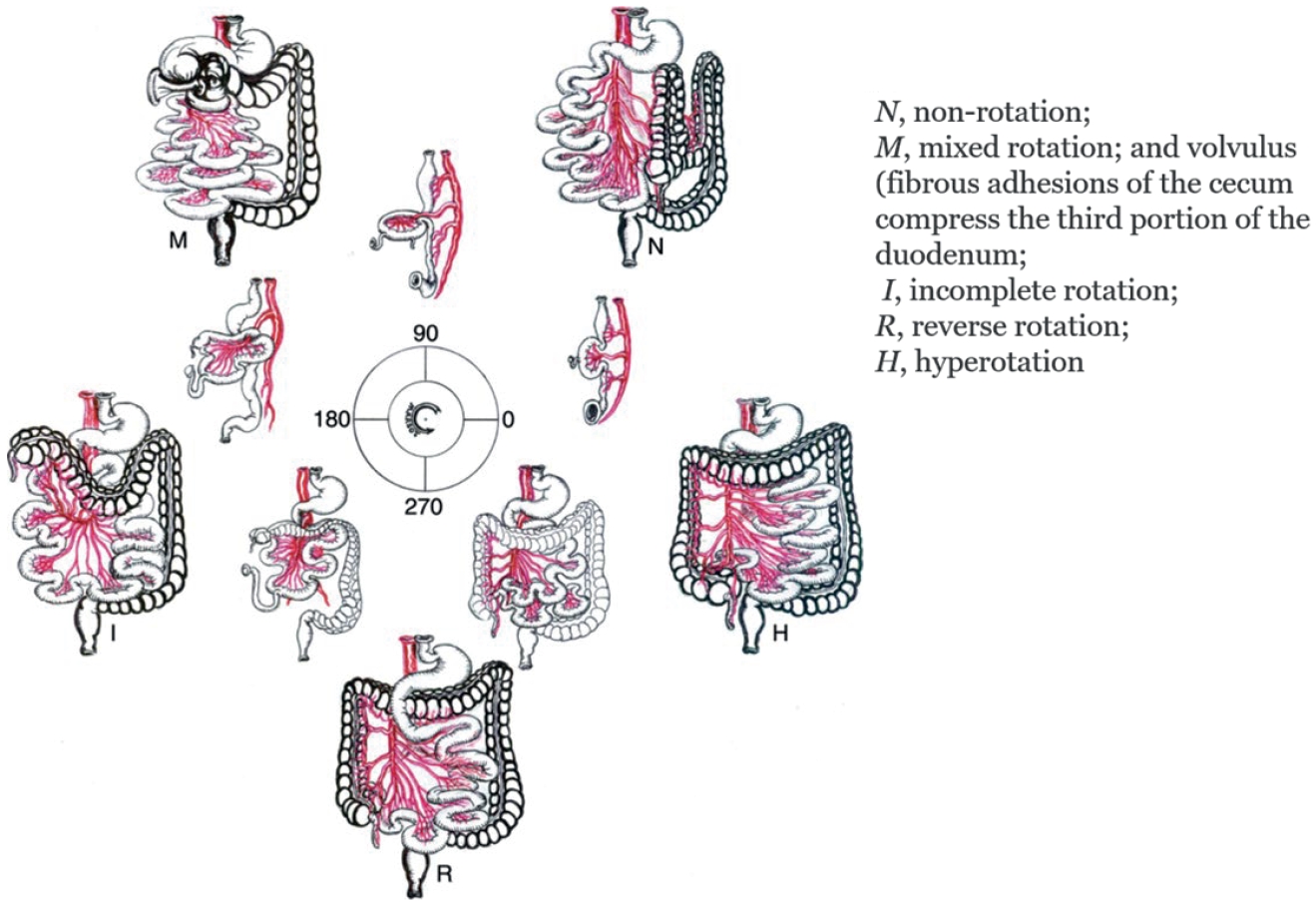
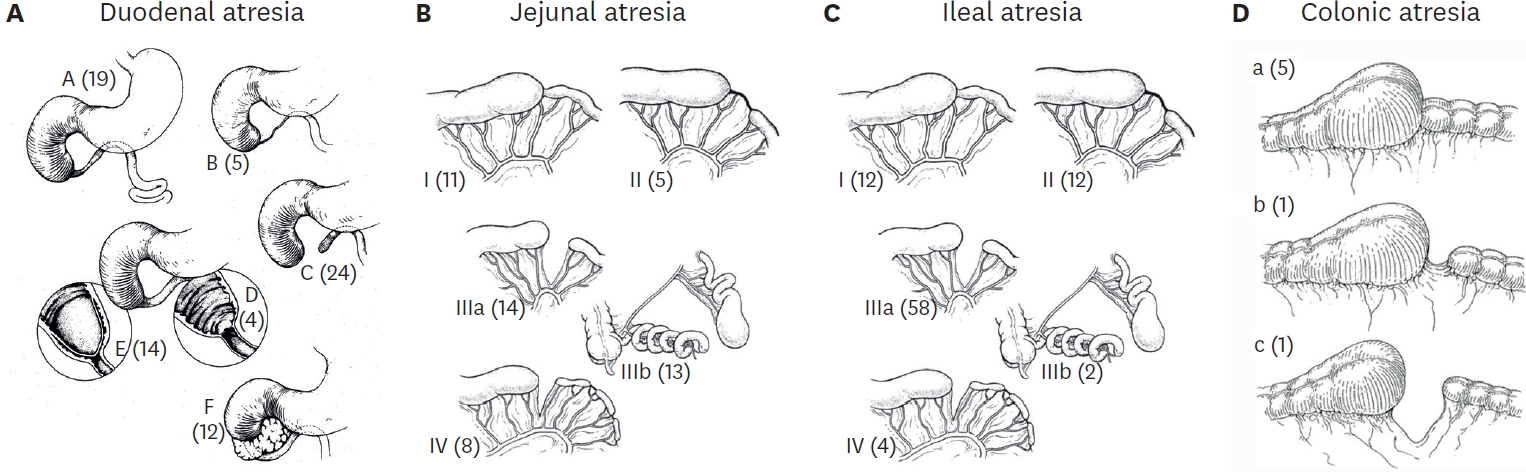
The Korean Association of Pediatric Surgeons (KAPS) performed a nationwide survey on sacrococcygeal teratoma in 2018.
The authors reviewed and analyzed the clinical data of patients who had been treated for sacrococcygeal teratoma by KAPS members from 2008 to 2017.
A total of 189 patients from 18 institutes were registered for the study, which was the first national survey of this disease dealing with a large number of patients in Korea. The results were discussed at the 34th annual meeting of KAPS, which was held in Jeonju on June 21–22, 2018.
We believe that this study could be utilized as a guideline for the treatment of sacrococcygeal teratoma to diminish pediatric surgeons' difficulties in treating this disease and thus lead to better outcomes.
Citations

We present an extremely rare case with double H-type tracheoesophageal fistulae identified with a time-lapse and repaired separately. A newborn male presented with cyanosis after breastfeeding. Contrast esophagogram demonstrated an H-type fistula, and then it was repaired in a standard fashion via right thoracotomy. When routine esophagogram was taken on postoperative day 10, another fistula was noticed at a level higher than the previous one. Bronchoscopy was performed to evaluate the lesion whether it was a recurred fistula or a second H-type fistula. However, it was so tiny that it was not visible with bronchoscopy. It was discovered only two months later when the fistula had grown up with the baby. The second H-type fistula was repaired through a cervical incision. Although double H-type fistulae are extremely rare, the possibility of another fistula, as well as recurrence, must be ruled out when symptom recurs after a definitive operation of an H-type fistula.
Citations

Gastric duplication is a rare anomaly which account for only 3.8% of all gastrointestinal duplication. Gastric duplications are usually cysticlesion without communication with lumen. Most frequent presentation is an abdominal mass with vomiting, mainly diagnosed within the first year of life. Surgical removal is necessary in all cases, and optimal timing for surgery is the time that diagnosis is made. However, prenatally diagnosed gastric duplication is getting more common, and determining timing for surgery is not easy due to absent or minimal symptoms just after birth. We experienced prenatally diagnosed gastric duplication in a female newborn baby that gastric duplication was suggested in 24th week of gestational age through prenatal ultrasonogram. Surgical removal was done at 3 months after birth, and showed good results. We think that natural history of gastric duplication and prevalent age of surgical disease which is similar to gastric duplication such infantile hypertrophic pyloric stenosis should be considered when timing of surgery on prenatally gastric duplication is decided.
Inguinal hernia is the most common disease treated by the pediatric surgeon. There are several controversial aspects of management 1)the optimal timing of surgical repair, especially for preterm babies, 2)contralateral groin exploration during repair of a clinically unilateral hernia, 3)use of laparoscope in contralateral groin exploration, 4)timing of surgical repair of cord hydrocele, 5)perioperative pain control, 6)perioperative management of anemia. In this survey, we attempted to determine the approach of members of KAPS to these aspects of hernia treatment. A questionnaire by e-mail or FAX was sent to all members. The content of the questionnaire were adapted from the “
Citations

Leveling colostomy with a frozen-section biopsy in a Hirschsprung's disease is an important factor for a successful procedure. Two neonatal cases of Hirschsprung's disease in the descending colon are reported. In both cases, loop ileostomy was established because of the unavailability of frozen-section biopsy on an emergency basis. At the time of definitive procedure of the first case, transition zone at the splenic flexure was noted and was compatible with the frozen section biopsy. In the second case, an unexpected longer resection at a higher level than transition zone was required because of the poor vascularity after dissection. In conclusion, a leveling colostomy should be selected as a choice in long-segment Hirschsprung's disease. Confirming preservation of the marginal artery of Drummond is particularly important in case of Hirschsprung's disease in the descending colon.
Visceral lipoma originating from the mesentery is very rare in childhood. A 29-month-old male presented with painless abdominal distension. Abdominal ultrasonography and CT revealed a huge multilobulated hypodense mass in the peritoneal cavity. Exploratory laparotomy showed a 26 × 25 × 5 cm sized encapsulated, lobulated, homogenous mass, which originated from the transverse mesocolon. Histologic examination revealed a lipoma. The postoperative course was uneventful.
Citations

A 10-year-old boy was admitted with blunt abdominal trauma by bike handle injury. The patient was operated upon for a generalized peritonitis due to pancreaticoduodenal injury. On opening the peritoneal cavity, complete transection of distal end of common bile duct and, partial separation between pancreas head and second portion of duodenum were found. Ligation of the transected end of the common bile duct, T-tube choledochostomy, and external drainage were performed. A pseudocyst was found around the head portion of the pancreas on the 7th postoperative day with CT. An internal fistula had developed between the pseudocyst and ligated common bile duct. The pseudocyst was subsided after percutaneous drainage. In the case of the undetermined pancreatic injury, percutaneous external drainage can be effective in treating the traumatic pancreatic pseudocyst in a pediatric patient.

