ABSTRACT
-
Purpose
Total proctocolectomy with ileal pouch-anal anastomosis (T-IPAA) in childhood is a surgical procedure mainly applied to familial adenomatous polyposis (FAP) or ulcerative colitis (UC), but it can be applied to non-FAP/non-UC disease (NFNU). Studies regarding the role of T-IPAA who underwent the operation in childhood, especially in terms of long-term gastrointestinal function, complications, and quality of life (QOL) are limited. The aim of this study was to evaluate the characteristics of patients receiving T-IPAA and to compare their bowel function outcomes and QOL.
-
Methods
Patients aged ≤18 years at the time of T-IPAA were included. Their medical records were retrospectively reviewed. Krickenbeck classification, Cleveland Clinic Incontinence (CCI) score, 36-item Short-form Health Survey Questionnaire, and Gastrointestinal Quality of Life Index were used for the evaluation of bowel function and QOL. The median follow-up period was 9.8 years.
-
Results
Of the 25 patients, 9 had FAP, 9 had UC, and 7 had NFNU. NFNU include 3 of Hirschsprung disease, 2 of intestinal neuronal dysplasia, and 2 of imperforate anus. The median age at T-IPAA was 17.8, 14.2, and 9.3 years for FAP, UC, and NFNU, respectively (p=0.001). Bowel function was satisfactory in terms of voluntary bowel movement (VBM), soiling, and constipation. VBM and constipation were not different between the groups, but soiling was most in NFNU (100%, p=0.047). However, QOL was best in the NFNU group in surveys (p=0.034 and 0.004, respectively).
-
Conclusion
T-IPAA could be safely applied not only for FAP and UC but also for other diseases in selective cases, with caution.
-
Keywords: Ileoanal pouches; Familial adenomatous polyposis; Ulcerative colitis; Pediatrics; Hirschsprung disease
INTRODUCTION
Total proctocolectomy with ileal pouch-anal anastomosis (T-IPAA) is a known standard operation in familial adenomatous polyposis (FAP) and ulcerative colitis (UC) [
12]. In adult patients with UC and FAP, studies on surgical outcomes and complications after T-IPAA reported generally good bowel function and gradually increasing pouch problems with longer follow-ups [
34567].
However, data regarding the role of T-IPAA in pediatric patients, especially in terms of long-term gastrointestinal function, complications, and quality of life (QOL) are limited [
8910]. T-IPAA remains a technically demanding procedure and may be associated with morbidity which may influence long-term pouch function and QOL. In addition, studies on T-IPAA due to diseases other than FAP or UC have been rarely conducted. To our knowledge, only a few studies in the English literature have reported the results of IPAA in pediatric non-FAP/non-UC disease (NFNU) [
9111213].
The aim of this study was to evaluate the characteristics of patients receiving T-IPAA for FAP, UC, and other diseases in childhood and to compare their bowel function outcomes and QOL.
METHODS
1. Study design
This study was performed in patients who underwent T-IPAA at age 18 or below in our tertiary hospital between June 1991 and December 2014. The study group comprised 25 patients, median age of T-IPAA was 14.1 years (range, 0.7–18.9). The underlying diseases for which T-IPAA was performed were FAP, UC, NFNU, including Hirschsprung disease (HD), intestinal neuronal dysplasia (IND), and imperforate anus (IA).
We retrospectively reviewed the medical records for the patients' age, sex, body weight, preoperative medication, operative methods, operation time, postoperative hospital stay, and postoperative complications. The median follow-up duration was 9.8 years (range, 2.1–25.9).
The current bowel function and QOL were analyzed prospectively using questionnaires and a retrospective chart review. Respondents to the questionnaires were patients aged ≥18 years and the guardians of patients aged <18 years. Of the 25 patients, 21 (88%) responded. Four patients were excluded from the evaluation because of current ostoma in 1 patient and missing questionnaire response in 3.
2. Bowel function and QOL evaluation of patient status
The Krickenbeck classification for postoperative results and the Cleveland Clinic Incontinence (CCI) score were used to evaluate bowel function. The Krickenbeck classification can evaluate voluntary bowel movement (VBM), soiling, and constipation [
14]. The CCI score consists of evaluations in 5 different situations where incontinence occurs. Each type of incontinence is rated on a scale from 0 (never) to 4 (always) to yield a total score that can range from 0 to 20, with higher scores indicating higher levels of incontinence [
15].
The 36-item Short-Form Health Survey Questionnaire (SF-36) and Gastrointestinal Quality of Life Index (GIQLI) were used to evaluate QOL [
1617]. Complications were classified as early (within 30 days after surgery) and late (30 days after surgery) complications.
Data were analyzed using SPSS version 20.0 (SPSS Inc., Chicago, IL, USA). Descriptive statistics were reported using median (range) for continuous variables and frequency (percent) for categorical variables. The nonparametric variance analysis was performed using the Kruskal-Wallis method, and t-tests were performed for mean comparisons. Correlations between variables were evaluated using the χ2 test. The α level was set at <0.05 for statistical significance. This study was approved by the Institutional Review Board (IRB) of our hospital (IRB No. 1707-053-867).
RESULTS
1. Demographics and clinical course
Nine patients with FAP, 9 with UC, and 7 with NFNU were treated. The median age at the time of T-IPAA was 14.1 years, and the oldest and youngest (17.8 and 9.3 years) patients were among those who underwent FAP and NFNU, respectively (p=0.001). Ileostomy was performed in all the patients except in 2 in the FAP group and 1 in the UC group. The median operation time was the longest at NFNU (301.8 minutes) and the lowest at UC (202 minutes), but not statistically significant. The median postoperative hospital stay was 19.3 days and was longest in the UC group (24 days, p=0.049;
Table 1). The differences in early and late complications among the 3 groups were not statistically different. In particular, pouchitis occurred in 11.1% of the FAP group and 22.2% of the UC, and did not occur in the NFNU, which was more likely to occur in the UC, but not statistically significant (
Table 2).
Table 1Demographics and operation-related data
Table 1
|
Variables |
Total |
FAP |
UC |
NFNU |
p-value |
|
No. of patients |
25 (100.0) |
9 (36.0) |
9 (36.0) |
7 (28.0) |
|
|
Male |
16 (64.0) |
5 (55.6) |
6 (66.7) |
5 (71.4) |
0.871 |
|
Age (yr) |
|
|
|
|
|
|
at diagnosis |
11.6 (0.2–18.7) |
16.6 (13.6–18.7) |
11.1 (5.1–13.7) |
5.8 (0.2–15.0) |
0.001 |
|
at T-IPAA |
14.1 (0.7–18.9) |
17.8 (15.1–18.9) |
14.2 (12.6–16.0) |
9.3 (0.7–15.4) |
0.001 |
|
Weight (kg) at T-IPAA |
42.6 (8.0–70.1) |
55.4 (36.7–67.1) |
41.9 (22.5–70.1) |
27.2 (8.0–43.0) |
0.103 |
|
Preoperative medication |
10 (40.0) |
1 (11.1) |
9 (100.0) |
0 |
0.001 |
|
Laparoscopic surgery |
3 (12.0) |
2 (22.2) |
0 |
1 (14.3) |
0.156 |
|
IPAA anastomosis method |
|
|
|
|
0.959 |
|
Hand-sewing |
13 (52.0) |
4 (44.4) |
5 (55.6) |
4 (57.1%) |
0.655 |
|
Using stapler |
12 (48.0) |
5 (55.6) |
4 (44.4) |
3 (42.9) |
0.712 |
|
Ileostomy formation |
22 (88.0) |
7 (77.8) |
8 (88.9) |
7 (100.0) |
0.411 |
|
Operation time (min) |
243 (145–415) |
224 (150–390) |
202 (145–340) |
301.8 (155–415) |
0.075 |
|
Postoperative hospital stays (day) |
19.3 (7–56) |
11 (7–23) |
24 (10–56) |
15.0 (9–46) |
0.049 |
|
Follow-up (yr) |
9.8 (2.1–25.9) |
8.1 (2.1–17) |
13.8 (6.3–25.9) |
6.9 (5.4–6.8) |
0.615 |
Table 2Complications
Table 2
|
Variables |
Total |
FAP |
UC |
NFNU |
p-value |
|
No. of patients |
25 (100.0) |
9 (36.0) |
9 (36.0) |
7 (28.0) |
|
|
Early |
6 (24.0) |
2 (22.2) |
4 (44.4) |
0 |
0.128 |
|
Fluid collection |
1 (4.0) |
0 |
1 (11.1) |
0 |
0.435 |
|
Wound complication |
1 (4.0) |
0 |
1 (11.1) |
0 |
0.435 |
|
Ileus |
4 (16.0) |
2 (22.2) |
2 (22.2) |
0 |
0.384 |
|
Internal herniation |
1 (4.0) |
0 |
1 (11.1) |
0 |
0.411 |
|
Late |
16 (64.0) |
8 (88.9) |
4 (44.4) |
4 (57.1) |
0.143 |
|
Wound complication |
3 (12.0) |
2 (22.2) |
0 |
1 (14.3) |
0.309 |
|
Perianal fistula |
3 (12.0) |
0 |
1 (11.1) |
2 (28.6) |
0.260 |
|
Rectovaginal fistula |
2 (8.0) |
0 |
2 (22.2) |
0 |
0.435 |
|
Anal stricture |
2 (8.0) |
0 |
2 (22.2) |
0 |
0.395 |
|
Ileus |
8 (32.0) |
5 (55.5) |
2 (22.2) |
1 (14.3) |
0.105 |
|
Pouchitis |
3 (12.0) |
1 (11.1) |
2 (22.2) |
0 |
0.175 |
2. Clinical features of the patients with NFNU
Of the patients with NFNU, 3 were diagnosed as having HD; 2, IND type B; and 2, IA with visceral neuropathy or hypoganglionosis. Operation indications were thoroughly investigated for each patient.
All HD patients were complicated cases, not just simple HD patients. One patient with rectosigmoid HD had septic shock with total colonic necrosis and had to undergo T-IPAA. The other 2 patients with HD were diagnosed as having total colonic aganglionosis and initially underwent Duhamel operation. After performing initial anastomosis in both patients, it was observed that the small bowel mesentery had torsion and was caught in the anastomosis line; therefore, pouch formation had to be conducted. The remaining 4 patients had persistent colonic dilatation and fecal incontinence before undergoing T-IPAA. In the final review, the diagnosis was IND type B in 2 patients, IA with visceral neuropathy of the colon in 1, and IA with hypoganglionosis with immature ganglion cells in 1. Owing to the difficulties in the diagnosis of IND, visceral neuropathy, and hypoganglionosis or “variant HD” [
18], these patients underwent a median of 4 operations (range, 1–9) before performing T-IPAA (
Table 3).
Table 3Evaluation of bowel functions by applying scoring methods
Table 3
|
Variables |
Total |
FAP |
UC |
NFNU |
p-value |
|
No. of patients |
21 (100.0) |
8 (38.1) |
7 (33.3) |
6 (28.6) |
|
|
Krickenbeck continence score |
|
|
|
|
|
|
Voluntary bowel movement |
20 (95.2) |
7 (87.5) |
7 (100.0) |
6 (100.0) |
0.287 |
|
Soiling (no) |
10 (47.6) |
5 (62.5) |
5 (71.4) |
0 |
0.047 |
|
|
Grade 1 |
8 (38.1) |
3 (37.5) |
1 (14.3) |
4 (66.7) |
0.394 |
|
|
Grade 2 |
1 (4.8) |
0 |
0 |
1 (16.7) |
0.287 |
|
|
Grade 3 |
2 (9.5) |
0 |
1 (14.3) |
1 (16.7) |
0.287 |
|
Constipation (no) |
1 (4.8) |
0 |
1 (14.3) |
0 |
0.368 |
|
|
Grade 1 |
18 (85.7) |
7 (87.5) |
6 (85.7) |
5 (83.3) |
0.977 |
|
|
Grade 2 |
2 (9.5) |
1 (12.5) |
0 |
1 (16.7) |
0.572 |
|
|
Grade 3 |
0 |
0 |
0 |
0 |
1.00 |
|
CCI score |
4.2 |
3.9 |
2.3 |
5.2 |
0.409 |
3. Bowel function outcomes
The questionnaires were administered to 8, 7, and 6 patients in the FAP, UC, and NFNU groups, respectively. In the Krickenbeck classification, VBM was observed in 20 of 21 patients, and differences among the groups were not significant. Fecal soiling was observed in 11 of 21 patients and was most frequent in the NFNU group (100%, p=0.047). Eight out of 11 patients with soiling were grade 1 (which happens occasionally). Two patients with soiling grade 3 (which is consistent) were in the FAP and NFNU groups. Twenty of the 21 patients had constipation, but 18 of them were grade 1, which was manageable by diet modification. The degree of incontinence evaluated on the basis of CCI scores was not significantly different among the groups (all <7), which means “good continence” (
Table 4).
Table 4Clinical features of NFNU patients
Table 4
|
Case |
Sex |
Diagnosis |
At IPAA operation |
Cause of total proctocolectomy with IPAA |
No. of operations before IPAA |
|
Age (yr) |
Weight (kg) |
|
1 |
M |
Hirschsprung's disease (RSA) |
13 |
29.8 |
Septic shock with total colonic necrosis |
3 |
|
2 |
M |
Intestinal neuronal dysplasia, type B |
12.7 |
36.9 |
Persistent colonic dilatation and fecal incontinence |
7 |
|
3 |
M |
Hirschsprung's disease (TCA) |
3.66 |
13.9 |
Duhamel anastomosis failure |
3 |
|
4 |
M |
Hirschsprung's disease (TCA) |
0.72 |
8 |
Duhamel anastomosis failure |
1 |
|
5 |
F |
Intestinal neuronal dysplasia, type B |
13.7 |
40 |
Persistent colonic dilatation and fecal incontinence |
9 |
|
6 |
M |
IA (RUF), Visceral neuropathy |
15.4 |
43 |
Persistent colonic dilatation and fecal incontinence |
4 |
|
7 |
F |
IA (RVF), Hypoganglinosis with immature ganglion cell |
6.5 |
18.6 |
Persistent colonic dilatation and fecal incontinence |
4 |
4. QOL
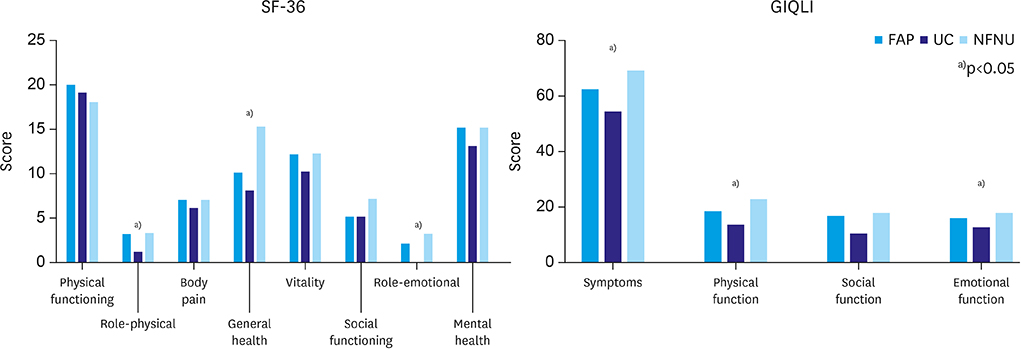
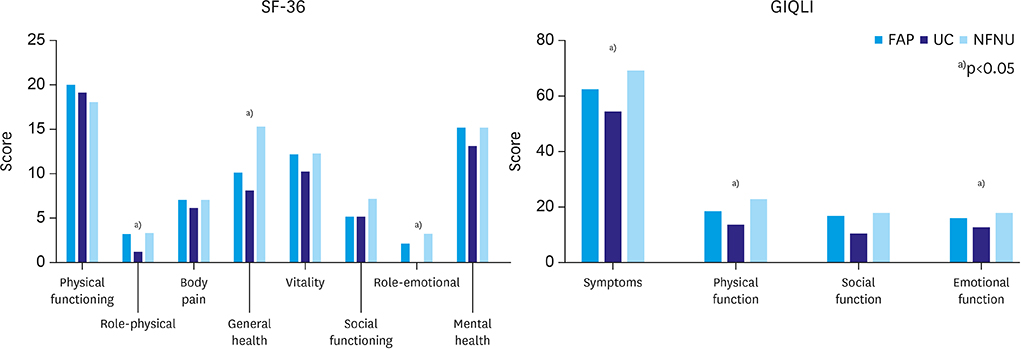
For analysis of QOL, the median SF-36 and GIQLI scores were 75 (range, 61–92) and 116 (range, 73–133), respectively, and showed significant differences among the groups. The best results were found in the NFNU group; and the worst results in the UC group (p=0.034 and 0.004, respectively;
Table 5). In the subgroup analysis of the SF-36 scores, 3 items of physical and emotional role functioning and general health perceptions showed differences between the groups. For these items, the NFNU and UC groups showed the best and worst results, respectively. In the GIQLI survey, the categories of gastrointestinal symptoms, physical function, and emotional function showed significant differences, and the NFNU group showed the best results (
Fig. 1).
Table 5Evaluation of quality of life by applying scoring system
Table 5
|
Variables |
Total |
FAP |
UC |
NFNU |
p-value |
|
SF-36 |
75 (61–92) |
74 (61–92) |
62 (52–82) |
78 (68–87) |
0.034 |
|
GIQLI |
116 (73–133) |
111 (91–125) |
89 (73–122) |
125 (113–133) |
0.004 |
Fig. 1
Detailed results of quality of life evaluation by questionnaires.
SF-36, Short-Form 36 Health Survey Questionnaire; GIQLI, Gastrointestinal Quality of Life Index; FAP, familial adenomatous polyposis; UC, ulcerative colitis; NFNU, non-familial adenomatous polyposis/non-ulcerative colitis disease.
DISCUSSION
IPAA, first described by Parks and Nicholls in 1978 [
19], has been the surgical approach of choice in medically refractory mucosal UC, indeterminate colitis, and FAP in adult patients. However, for pediatric patients, straight pull-through was considered to be superior to pouch formation in terms of reducing the risk of pouchitis, until the mid-1990s [
20]. Since the publication of favorable outcomes of IPAA in pediatric patients with UC and FAP, IPAA has also been the standard method of operation in children [
2122].
In terms of surgical indications, pediatric patients with UC undergo surgical corrections for medically uncontrolled status, severe bleeding, obstruction, cancer risk, perforation, and side effects of chronic medical therapy. In children with FAP, operation is indicated to reduce the life-long risk of developing cancer. Pediatric patients who undergo T-IPAA for FAP and UC are usually in their mid to late teens [
9].
The studies on pediatric patients with FAP and UC have reported postoperative outcomes, including complications. Fonkalsrud [
11] evaluated 116 pediatric patients who underwent T-IPAA and found that complications occurred in 41% of the patients, of which 15.5% had pouchitis, which occurred only in the patients with UC. This study followed up the patients for a mean of 7.1 years, and 92.2% of the patients reported good progress. In another recent report, 41 patients aged 2 to 17 years who had inflammatory bowel disease and FAP underwent IPAA, of which 9 (21.9%) developed pouchitis and 3 (7.3%) had pouch failure during 22 months of follow-up [
23]. In a recent systematic review article on T-IPAA in childhood, the incidence of chronic pouchitis was reported to be 13.2% [
24]. In the study of adults, the incidence of pouchitis was known to range from 7% to 46% [
25]. In this present study, pouchitis occurred in 12% of patients during median 9.8 years of follow-up.
T-IPAA has been performed rarely in pediatric patients with diseases other than FAP or UC. A study reported the results of restorative proctocolectomy with J-pouch ileoanal anastomosis applied in 8 newborn infants with total colonic aganglionosis. In this study, IPAA was performed at a median age of 1.1 months. For the short-term bowel function outcome evaluated at a median age of 3.2 years, the overall satisfaction with the operative results was high [
12]. Rintala and Lindahl [
13] reported the results of T-IPAA in 10 patients with HD who underwent T-IPAA at a median age of 1.5 years. No pouchitis-like symptoms occurred during the 3-year follow-up period, and 3 patients had episodes of postoperative enterocolitis. In addition, all the patients aged >3 years were reported to be continent.
In our study, T-IPAA was applied in 25 pediatric patients between June 1991 and December 2014, and their underlying diseases were UC, FAP, HD, IND, and IA. For UC and FAP, T-IPAA is a standard procedure for surgical treatment, and our center followed the indications such as medically intractable status or increased risk of malignancy for treating the patients. For patients with NFNU, the operation indications were investigated for each patient thoroughly, and T-IPAA was performed because bowel continuity could not be maintained with the colon for various reasons.
Bowel function after total T-IPAA was satisfactory because VBM was identified in 20 of 21 patients, of which 18 had no soiling or grade 1 soiling, and 90.5% had no constipation or showed improvement with diet modification. CCI score also showed good continence. The significantly more frequent occurrence of soiling in the NFNU group may have been due to multiple prior operations that caused injuries in the perianal area and could be the reason for the highest rate of fecal soiling in the group.
QOL analysis revealed the best score in the NFNU group, contrary to the bowel function outcomes. This could imply that patients with NFNU with prior co-morbidities that persisted before the IPAA procedure may have enhanced the satisfaction after T-IPAA, as seen in the history of these patients with NFNU.
The UC group showed worst QOL in our study. This result could be explained by many reasons, one of which is the use of medications for treating underlying diseases. A research study that included patients with UC and FAP with IPAA for a long-term follow-up of 10 years reported that long-term steroid used before surgery in patients with UC prolonged the time to normalize bowel function [
26]. In our study, the UC group used more preoperative steroids than the FAP or NFNU group. This may have also influenced the poor QOL scores of the patients in the UC group.
The limitations of our study include its retrospective nature and small study population, and the recall bias during the collection of information through the questionnaire survey.
T-IPAA was mainly applied for FAP or UC, but could also be performed when the colon could not be used for anastomosis for various reasons in children. Postoperative bowel function was satisfactory in terms of VBM, soiling, and constipation, but fecal soiling was more frequently observed in the patients with NFNU, possibly because of multiple operations before T-IPAA. When the QOL was surveyed, the NFNU group showed the best results and UC group showed the worst results, contrary to the bowel function outcomes. Therefore, T-IPAA could be safely applied not only for FAP and UC, but also for other diseases such as HD, IND, or IA in selective cases, with caution.
NOTES
-
The abstract of this article was presented at the Pacific Association of Pediatric Surgeons 51st Annual Scientific Meeting in Sapporo, Japan, on May 13–17, 2018.
-
No potential conflict of interest relevant to this article was reported.
REFERENCES
- 1. Tudyka VN, Clark SK. Surgical treatment in familial adenomatous polyposis. Ann Gastroenterol 2012;25:201-206.
- 2. Ross H, Steele SR, Varma M, Dykes S, Cima R, Buie WD, et al. Practice parameters for the surgical treatment of ulcerative colitis. Dis Colon Rectum 2014;57:5-22.
- 3. Fazio VW, Kiran RP, Remzi FH, Coffey JC, Heneghan HM, Kirat HT, et al. Ileal pouch anal anastomosis: analysis of outcome and quality of life in 3707 patients. Ann Surg 2013;257:679-685.
- 4. Hahnloser D, Pemberton JH, Wolff BG, Larson DR, Crownhart BS, Dozois RR. Results at up to 20 years after ileal pouch-anal anastomosis for chronic ulcerative colitis. Br J Surg 2007;94:333-340.
- 5. Tekkis PP, Lovegrove RE, Tilney HS, Smith JJ, Sagar PM, Shorthouse AJ, et al. Long-term failure and function after restorative proctocolectomy - a multi-centre study of patients from the UK National Ileal Pouch Registry. Colorectal Dis 2010;12:433-441.
- 6. Tulchinsky H, Hawley PR, Nicholls J. Long-term failure after restorative proctocolectomy for ulcerative colitis. Ann Surg 2003;238:229-234.
- 7. Uchino M, Ikeuchi H, Sugita A, Futami K, Watanabe T, Fukushima K, et al. Pouch functional outcomes after restorative proctocolectomy with ileal-pouch reconstruction in patients with ulcerative colitis: Japanese multi-center nationwide cohort study. J Gastroenterol 2018;53:642-651.
- 8. Lillehei CW, Leichtner A, Bousvaros A, Shamberger RC. Restorative proctocolectomy and ileal pouch-anal anastomosis in children. Dis Colon Rectum 2009;52:1645-1649.
- 9. Ozdemir Y, Kiran RP, Erem HH, Aytac E, Gorgun E, Magnuson D, et al. Functional outcomes and complications after restorative proctocolectomy and ileal pouch anal anastomosis in the pediatric population. J Am Coll Surg 2014;218:328-335.
- 10. Stavlo PL, Libsch KD, Rodeberg DA, Moir CR. Pediatric ileal pouch-anal anastomosis: functional outcomes and quality of life. J Pediatr Surg 2003;38:935-939.
- 11. Fonkalsrud EW. Long-term results after colectomy and ileoanal pull-through procedure in children. Arch Surg 1996;131:881-885.
- 12. Hukkinen M, Koivusalo A, Rintala RJ, Pakarinen MP. Restorative proctocolectomy with J-pouch ileoanal anastomosis for total colonic aganglionosis among neonates and infants. J Pediatr Surg 2014;49:570-574.
- 13. Rintala RJ, Lindahl HG. Proctocolectomy and J-pouch ileo-anal anastomosis in children. J Pediatr Surg 2002;37:66-70.
- 14. Holschneider A, Hutson J, Peña A, Beket E, Chatterjee S, Coran A, et al. Preliminary report on the International Conference for the Development of Standards for the Treatment of Anorectal Malformations. J Pediatr Surg 2005;40:1521-1526.
- 15. Jorge JM, Wexner SD. Etiology and management of fecal incontinence. Dis Colon Rectum 1993;36:77-97.
- 16. Eypasch E, Williams JI, Wood-Dauphinee S, Ure BM, Schmülling C, Neugebauer E, et al. Gastrointestinal Quality of Life Index: development, validation and application of a new instrument. Br J Surg 1995;82:216-222.
- 17. Ware JE Jr, Sherbourne CD. The MOS 36-item short-form health survey (SF-36). I. Conceptual framework and item selection. Med Care 1992;30:473-483.
- 18. Puri P, Gosemann JH. Variants of Hirschsprung disease. Semin Pediatr Surg 2012;21:310-318.
- 19. Parks AG, Nicholls RJ. Proctocolectomy without ileostomy for ulcerative colitis. BMJ 1978;2:85-88.
- 20. Coran AG. A personal experience with 100 consecutive total colectomies and straight ileoanal endorectal pull-throughs for benign disease of the colon and rectum in children and adults. Ann Surg 1990;212:242-248.
- 21. Nyam DC, Brillant PT, Dozois RR, Kelly KA, Pemberton JH, Wolff BG. Ileal pouch-anal canal anastomosis for familial adenomatous polyposis: early and late results. Ann Surg 1997;226:514-521.
- 22. Rintala RJ, Lindahl H. Restorative proctocolectomy for ulcerative colitis in children--is the J-pouch better than straight pull-through? J Pediatr Surg 1996;31:530-533.
- 23. Diederen K, Sahami SS, Tabbers MM, Benninga MA, Kindermann A, Tanis PJ, et al. Outcome after restorative proctocolectomy and ileal pouch-anal anastomosis in children and adults. Br J Surg 2017;104:1640-1647.
- 24. Tan Tanny SP, Yoo M, Hutson JM, Langer JC, King SK. Current surgical practice in pediatric ulcerative colitis: a systematic review. J Pediatr Surg 2018;Sep. 07. [Epub].
- 25. Dalal RL, Shen B, Schwartz DA. Management of pouchitis and other common complications of the pouch. Inflamm Bowel Dis 2018;24:989-996.
- 26. Raviram S, Rajan R, Sindhu RS, Bonny N, Kuruvilla AP, Subhalal N. Quality of life, social impact and functional outcome following ileal pouch-anal anastomosis for ulcerative colitis and familial adenomatous polyposis. Indian J Gastroenterol 2015;34:252-255.
 , Joong Kee Youn1
, Joong Kee Youn1 , Soo-Hong Kim3
, Soo-Hong Kim3 , Kyu Joo Park4
, Kyu Joo Park4 , Seung-Yong Jeong4
, Seung-Yong Jeong4 , Sung-Eun Jung1
, Sung-Eun Jung1 , Kwi-Won Park5
, Kwi-Won Park5 , Hyun-Young Kim1
, Hyun-Young Kim1