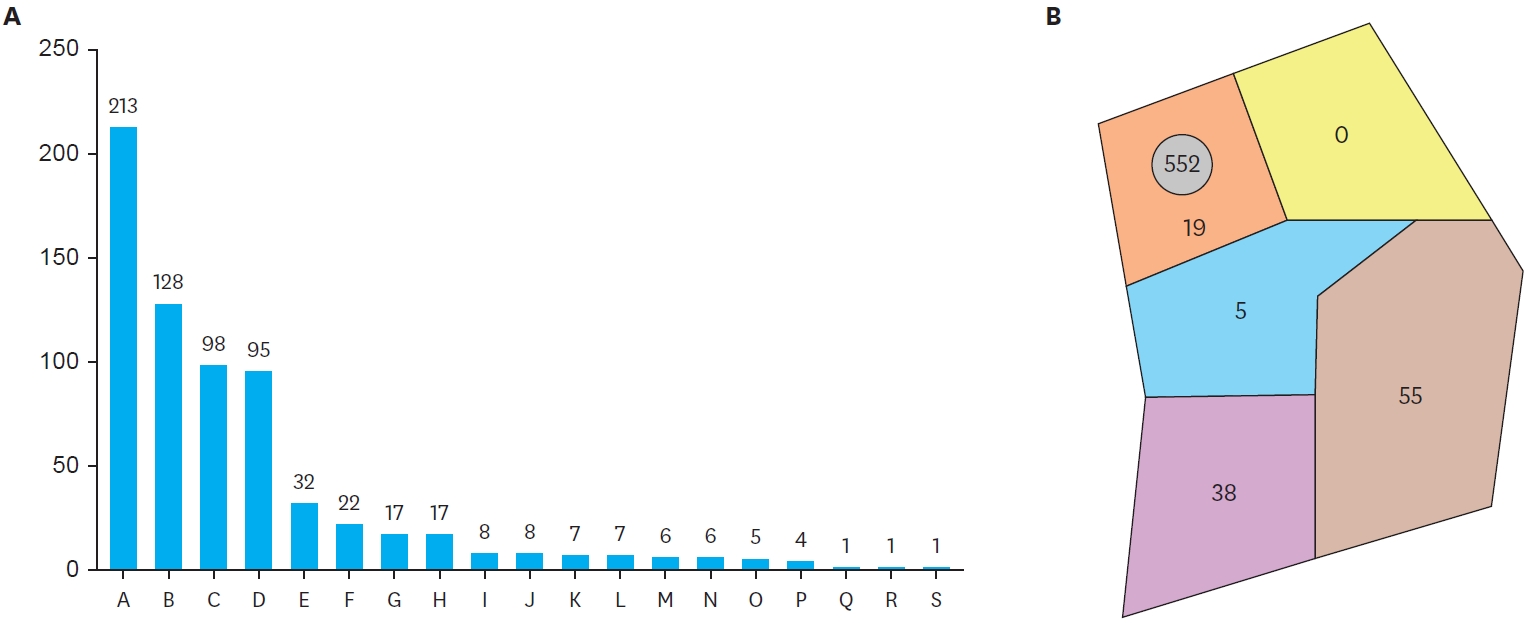
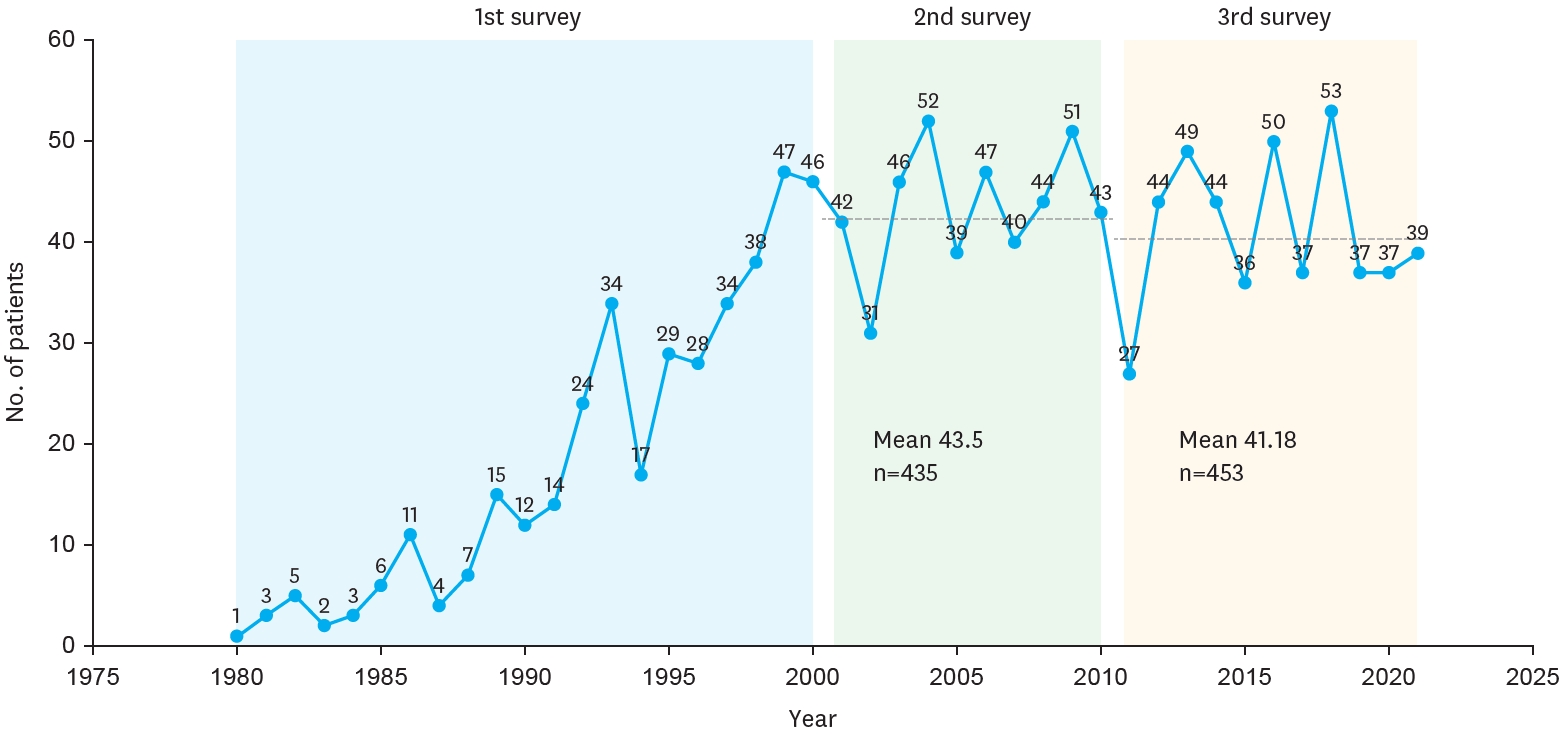
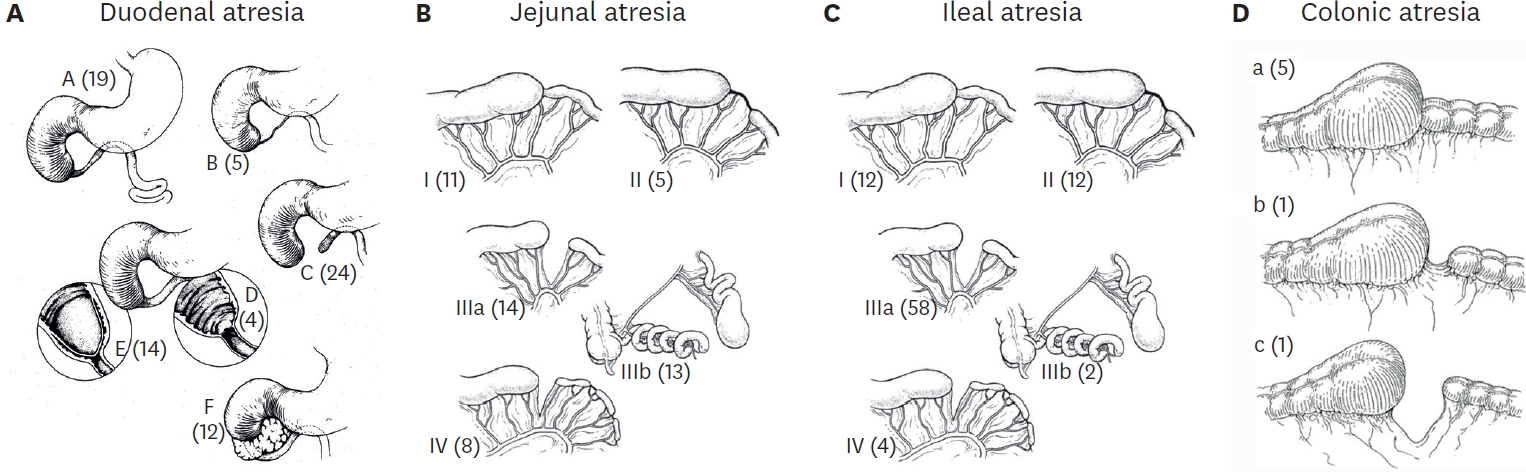
The Korean Association of Pediatric Surgeons (KAPS) performed a nationwide survey on sacrococcygeal teratoma in 2018.
The authors reviewed and analyzed the clinical data of patients who had been treated for sacrococcygeal teratoma by KAPS members from 2008 to 2017.
A total of 189 patients from 18 institutes were registered for the study, which was the first national survey of this disease dealing with a large number of patients in Korea. The results were discussed at the 34th annual meeting of KAPS, which was held in Jeonju on June 21–22, 2018.
We believe that this study could be utilized as a guideline for the treatment of sacrococcygeal teratoma to diminish pediatric surgeons' difficulties in treating this disease and thus lead to better outcomes.
Citations

Varicose veins requiring operative treatment have been more common recently, but there are not enough studies among children dermographics because most patients belong to the adult population. We concentrated on varicose vein of under 18 years old, and here intend to report cases of our clinical experiences.
From January 2003 until December 2014, there were 6 children under 18 years old who required varicose vein management. Data was collected by the investigation of medical records retrospectively, including preoperative symptoms, diagnostic tools, treatment methods, results of treatment, and complications.
The mean age was 11 years (range, 3-17 years), and gender ratio was 1:2 (2 male, 4 female). The involved legs were on the right in 3 cases, on the left in 2 cases, and on both in 1 case. The most common symptoms were venous bulging and tortuosity in 6 cases, and other symptoms were Klippel-Trenaunay-Weber syndrome in 2 cases, pain and fatigue in 1 case, port-wine stain in 1 case, and telangiectasia in 1 case. Duplex sonography was performed to confirm venous reflux in all cases. The additional venography was performed to check for anatomical variation in 1 case, and three-dimensional CT in 2 cases. Treatments were high ligation and stripping in 3 cases, and endovenous laser therapy in 3 cases. Additionally, remnant varicosities after first operations were treated by endovenous laser therapy in all cases. During the mean postoperative follow-up period of 60 months, complications included edema of the foot and petechia in 2 cases each, and were not severe.
Operative treatments including high ligation and stripping, and endovenous laser therapy are very effective for the management of varicose vein in the pediatric population, with improvements in quality of life including relief of symptoms and management of the cosmetic aspect.
Traumatic injury is one of the leading causes of morbidity and mortality in children. This is a clinical review of pediatric blunt abdominal trauma. A retrospective analysis of the 112 children with blunt abdominal trauma aged 15 years or less treated at the Department of Pediatric Surgery, Chonbuk National University Hospital was performed. The analysis included age, sex, injury mechanism, number and site of the injured organ, management and outcomes. The average age of occurrence was 7.6 years, and the peak age was between 6 and 8 years. There was a male preponderance with a male to female ratio of 2.3:1. The most common cause of blunt abdominal trauma was traffic accidents (61.6%), principally involving pedestrians (79.7%). The accident prone times were between 8:00 AM and 8:00 PM, the weekends (40.2%), and the winter respectively. Thirthy-five patients (31.2%) had multiple intra-abdominal organ injuries and the most common injured organ was the liver. Seventy-four cases (66.1%) were managed non-operatively and eleven cases (9.8%) expired. Of the patients who were treated surgically or were to be operated on one patient died before surgery, the remainder died during or after surgery. Risk factors such as number of injured organ, systolic and diastolic blood pressure, and trauma scores by Glasgow coma scale (GCS), Pediatric trauma score (PTS), revised trauma score (RTS), injury severe score (ISS), TRISS were significantly correlated with mortality rate.
Citations

Inguinal hernia is one of the most common surgical diseases in pediatric patients. But the management of the side opposite the clinically apparent inguinal hernia, the “silent side” is controversial. Four hundred fifty-eight cases of pediatric inguinal hernias, operated by one pediatric surgeon at the Divisionof Pediatric Surgery, Department of Surgery, Chonbuk National University Hospital from January 1998 to December 2002, were reviewed retrospectively to determine the characteristics and significances of the silk-glove test on the side opposite the clinically apparent inguinal hernia. Males were preponderant as 2.8:1. Allhernias were of the indirect type and were repaired by high ligation of the sac. There were 238 (52.0%) right sided hernias, 160 (35.0%) were on the left and 60 (13.0%) were bilateral. The number of patients with a positive silk-glove sign on the contralateral side was 158(39.7%), and 133 of these had a contralateral patent processus vaginalis. Positive predictive value of Silk-glove test was 84.2% (133/158). The silk-glove test is a simple, safe, and relatively accurate method for contralateral exploration in the unilateral inguinal hernias in children.
Citations

Ovarian cyst is found in 32% of necropsies in neonates, and can be visualized during gestation by ultrasonography. The clinical evolution of these cysts is variable, but in most cases the prognosis is favorable. Ovarian torsion, bleeding, rupture, and peritonitis have been described as complications. We report a newborn girl with torsion of ovarian cyst. A cystic mass measuring 41.9x31.9 mm on left side of abdomen was identified at 32 weeks of gestation by fetal ultrasonography. Surgery was performed after birth.
A total of 30 cases of the peptic ulcer in children, who underwent operations from January 1981 to December 1995 because of complications at Department of the Surgery, Chonbuk National University Medical School, is reviewed. Twenty-three were males (76.7%), 7 females (23.3%) and male was preponderant at 3.3:1. There were 25 cases (83.3%) age 10 to 15 years, 3 (10.0%) between 2 and 9 years, and 2 (6.7%) below 2. The ulcer was located at duodenum in 27 (90.0%), and at stomach in 3 cases (10.0%). Complications were perforation in 19 cases (63.3%), pyloric obstruction in 9 (30.0%) and bleeding in 2 (6.7%). For perforation, truncal vagotomy with pyloroplasty was done in 11 cases, truncal vagotomy with hemigastrectomy and gastrojejunostomy in 6, and simple closure in 2 cases. For obstruction, truncal vagotomy with hemigastrectomy and gastrojejunostomy was done in 5, and truncal vagotomy and pyloroplasty in 3 cases. For bleeding lesions, truncal vagotomy and pyloroplasty was performed in 2 cases. Ten postoperative complications developed in 9 patients; adhesive ileus in 5, recurrence in 2, pneumonia 2, and wound seroma 1 case. One patient developed a primary duodenal perforation and another a recurrent obstruction. Both of patients had symptoms for more than 3 years and were treated with truncal vagotomy and pyloroplasty for the primary operations. Hospital stay was 11.5 days for the patient with perforated ulcer, 11.0 days for the patient with pyloric obstruction, and 14.5 days for the child with bleeding. Average hospital period was 11.6 days. To reduce recurrences after operation, extensive procedure such as distal gastrectomy with vagotomy at the first operation should be considered in case with severe complication or with patients who have been symptomatic for long periods.
A 4-year-old female with acute lower abdominal pain was admitted with the diagnosis of periappendiceal abscess made by ultrasonography. At laparotomy, the appendix was normal, but the left ovary was twisted and necrotic. Appendectomy and left salpingo-oophorectomy were performed. The pathology of the appendix was normal, and the left tube and ovary were ischemic and had hemorrhagic necrosis. Pediatric adnexal torsion may be difficult to diagnosis clinically. Sonography is the preferred imaging study. It usually confirms a pelvic mass but may not establish the diagnosis. The correct diagnosis of adnexal torsion is often made at exploration. The most common erroneous diagnosis is acute appendicitis or periappendiceal abscess. Therapy for adnexal torsion remains controversial. While extirpation has been the standard of treatment in the past, there are current proponents of conservative therapy with adnexal sparing. Early diagnosis may lead to more frequent salvage of affected adnexa.
The purpose of our study was to evaluate children who underwent hepatic resection for primary malignant hepatic tumor in the period from January 1994 to December 2001. A total of 8 patients, seven with hepatoblastoma (HB) and one with hepatocellular carcinoma (HCC). were studied. One HCC was respectable at the initial diagnosis, but five cases of unresectable HB received two cycles of transarterial chemoembolization (TACE) before operation. One patient with an unresectable HB with bone marrow metastasis was operated after one cycle of TACE and one cycle of systemic chemotherapy based on CCG-823F protocol. All 6 patients who underwent TACE and neoadjuvant chemotherapy showed marked redcuction in tumor volume and a clear outline of the lesion. Major complication was not noticed. Mean alpha-fetoprotei (alpha-FP) level at diagnosis, after neoadjuvant chemotherapy and after postoperative chemotherapy was 9,818 (42-35,350), 664, and 10.1 ng/mL, respectively. Half life of the alpha-FP after complete resection was 5.1 days (3.0-8.7 days). Median follow up period was 57.1 months (10-97 months) and all the patients are alive with NED. In conclusion, preoperative chemotherapy, especially TACE, is effective, safe, and useful to treat initially unresectable hepatoblastoma, and serial level of the serum alpha-FP is a useful tumor marker for diagnosis and monitoring therapeutic responses.
Although intraperitoneal teratomas are rare, teratomas of the greater omentuma are seldom reported. A single case of omental teratoma with torsion in a 26-month-old girl is reported. The patient presented with abdominal pain and a palpable mass. Ultrasonography and CT of the abdomen showed a large cystic mass with a non homgenious solid component composed of fat and calcification. The lesion was surgically excised. Pathology revealed a mature omental teratoma. The hospital course was uneventful.
Idiopathic small bowel ulceration distal to the duodenum is rare. Less than 5 % of the reported cases were in children. In the majority of the patients, a single ulcer of unknown cause is found in the jejunum or ileum. The diagnosis is difficult and usually made at the time of surgical exploration for complications, such as perforation, hemorrhage or obstruction. We treated a pediatric patient with perforation of an idiopathic ileal ulceration. The child was an ll-year-old boy who sustained blunt abdominal trauma. The involved ileal segment was resected. Pathologic findings were compatible with idiopathic small bowel ulceration. The clinical and pathological aspects of idiopathic ulcerations are discussed, and the literature reviewed.

