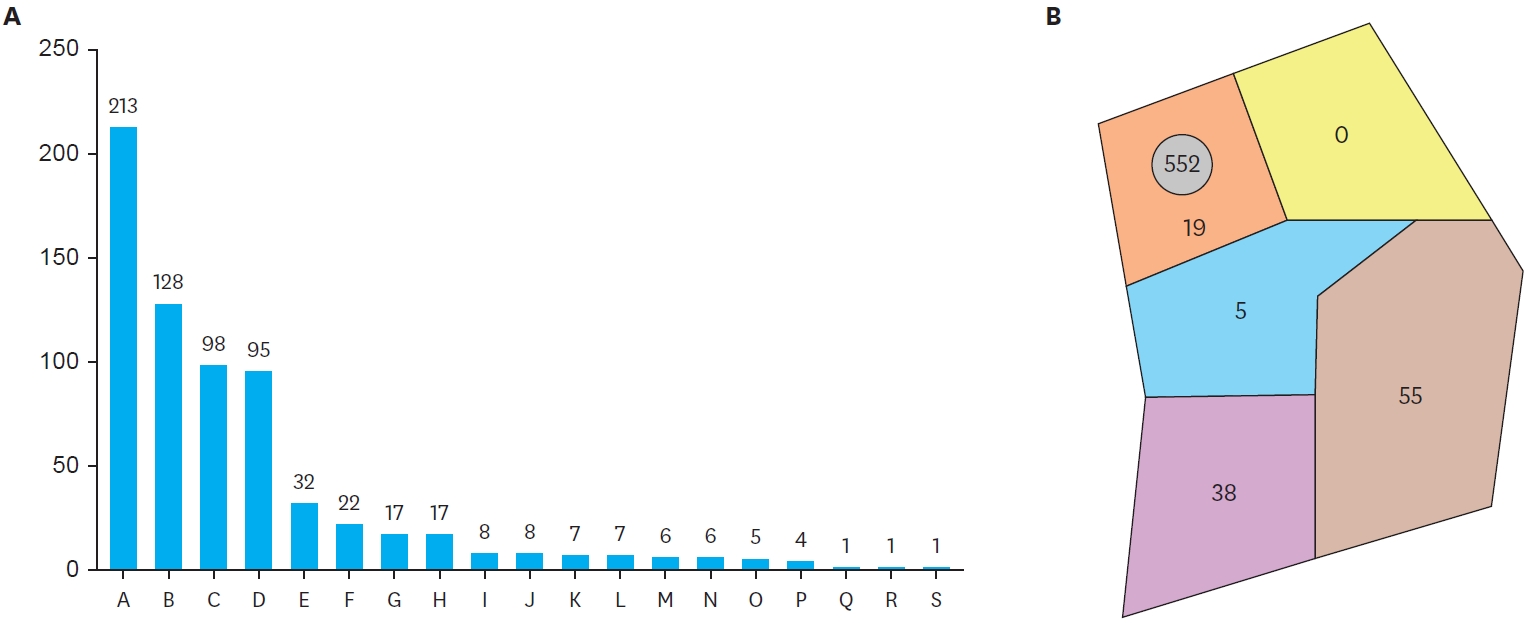
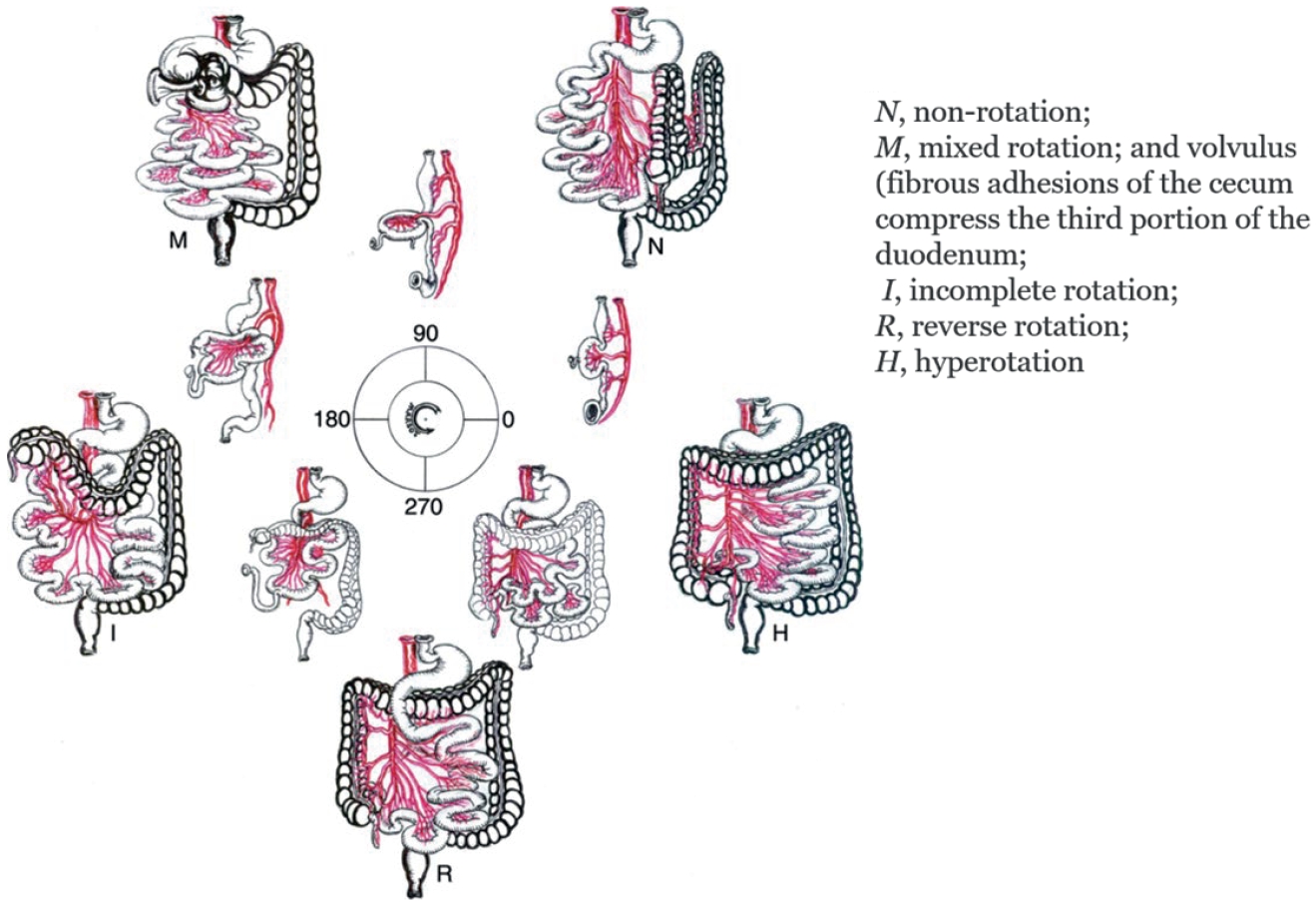
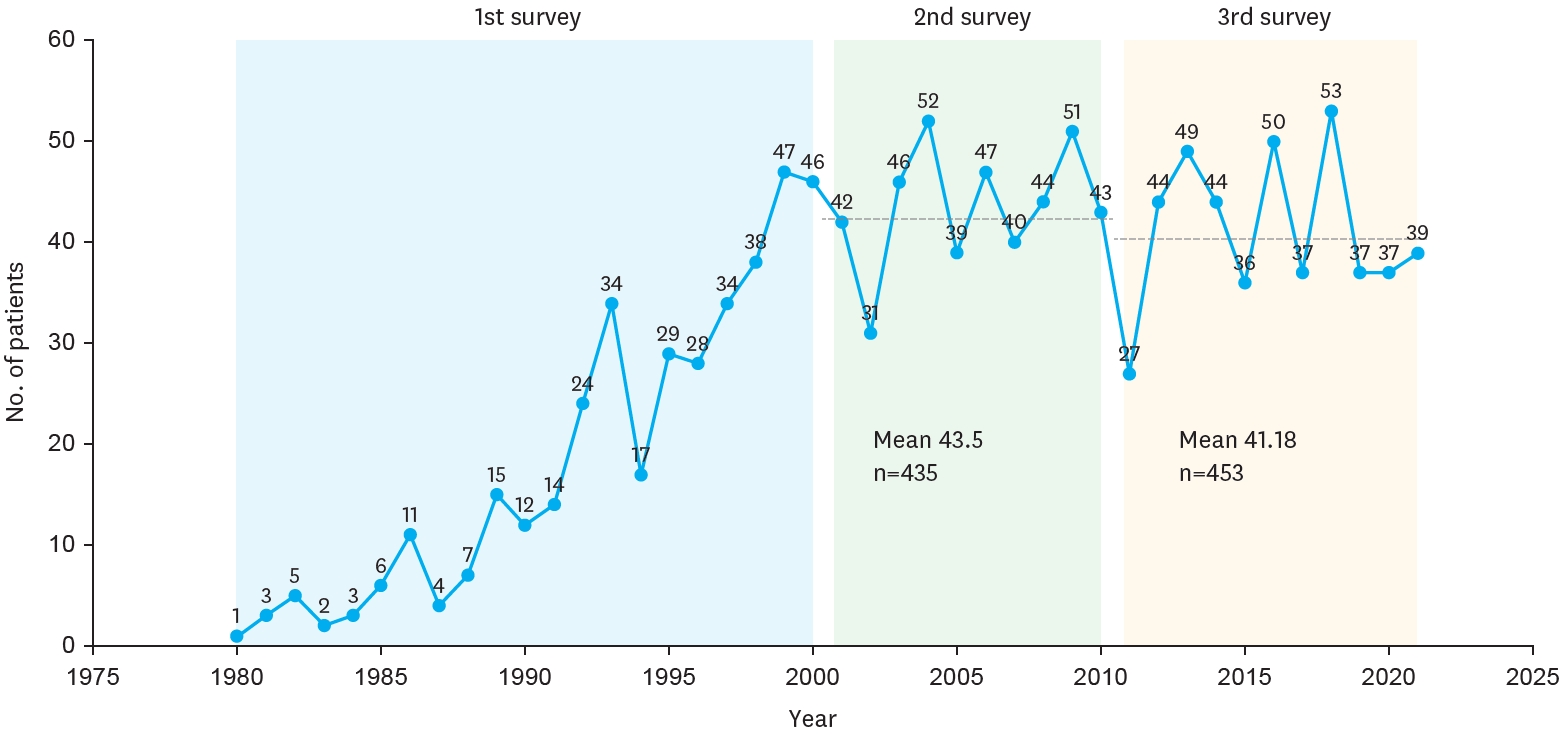
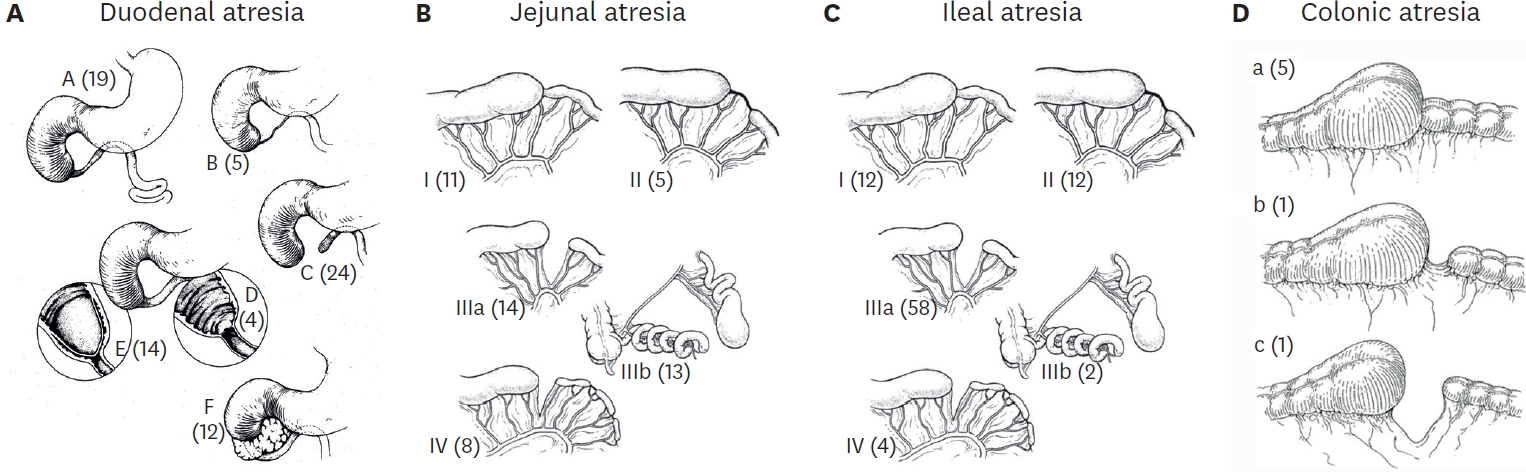
The Korean Association of Pediatric Surgeons (KAPS) performed a nationwide survey on sacrococcygeal teratoma in 2018.
The authors reviewed and analyzed the clinical data of patients who had been treated for sacrococcygeal teratoma by KAPS members from 2008 to 2017.
A total of 189 patients from 18 institutes were registered for the study, which was the first national survey of this disease dealing with a large number of patients in Korea. The results were discussed at the 34th annual meeting of KAPS, which was held in Jeonju on June 21–22, 2018.
We believe that this study could be utilized as a guideline for the treatment of sacrococcygeal teratoma to diminish pediatric surgeons' difficulties in treating this disease and thus lead to better outcomes.
Citations

Early suspicion is essential in diagnosing pyriform sinus cysts. We report two neonatal cases of pyriform sinus cysts presented as neck masses. The first case presented as a right neck mass, which made it more difficult to suspect a pyriform sinus cyst considering the prevalence of left sided cysts. Surgical resection was done in both cases and anatomical investigation suggested both to originate from the fourth branchial pouch. Detection of air bubble containing mass on imaging studies can aid early diagnosis and early use of gastric tube feeding can facilitate treatment by preventing milk contamination which may result in infection of the sinus cyst.
Citations

The use of CT as a diagnostic tool in pediatric acute appendicitis is increasing because of its high sensitivity and specificity. However, due to both the serious concerns about radiation of CT and the convenience and reasonable cost of ultrasound (US) examination, US has value on the initial diagnosis of acute appendicitis despite of the lower sensitivity in children. The purpose of this study was to examine the factors that affect the rate of false negative diagnosis of the ultrasound from the patients who received laparoscopic appendectomy.
The pediatric appendectomy cases from 2002 to 2013 in Yeouido St. Mary's Hospital have been reviewed through the medical records. We included patients who underwent an initial screening by ultrasound examination.
Among 181 patients, 156 patients were the sono-positive group and 25 patients were sono-negative group. There is no significant difference in ages, genders, physical examination findings and white blood cell count between the two groups. But, the degree of inflammation of appendicitis (simple, 58.3% vs. 32.0%; complicated, 41.7% vs. 68.0%) and the appendix position (antececal, 85.0% vs. 12.0%; retrocecal, 13.7% vs. 44.0%; pelvic, 1.3% vs. 44.0%) were significantly different between the two groups (sono-positive group vs. sono-negative group; p<0.05).
The position of the appendix may act as a factor that causes an error in the diagnostic ultrasound, especially, in the retrocecal type and the pelvic type with the higher risk of necrosis or perforation.
Citations

Use of laparoscopic appendectomy (LA) for perforated appendicitis (PA) in children remains controversial because of the development of postoperative intra-abdominal abscess formation. We developed the irrigation method for the prevention of abscess formation after LA performed for PA in children with severe panperitonitis. We called it ‘the shaking irrigation’. The object of this study was to analyze the efficacy of this irrigation method. All cases of PA with severe panperitonitis in children that underwent LA with massive shaking irrigation and drainage between June 2003 and December 2007 were studied retrospectively. We included only PA with panperitonitis and large amounts of purulent ascites throughout the abdomen as well as an inflamed small bowel with ileus. Thirty-four children were involved in this study. The mean patient age was eight years. The mean amount of irrigation fluid was 8.2L (range: 4-15L). The mean operative time was 89.5 min. The mean length of the hospital stay was 5.1 days. There were no postoperative intra-abdominal abscesses. There was no conversion to open surgery. In conclusion, Use of LA in PA with severe panperitonitis in children is safe and effective. Massive shaking irrigation and abdominal drainage appears to prevent intra-abdominal abscesses after LA for PA with panperitonitis.
To evaluate the long-term prognosis of biliary atresia after Kasai operation, a total of 14 patients (of the 41 patients operated upon from 1982 to 1997), who had been followed up for more than 10 years, were included in this retrospective study. Eleven out of 14 patients survived with their native livers, and their data analyzed for age at operation, clearing time of jaundice, histological outcome, postoperative complications, effectiveness after the application of an intussusception anti-reflex valve, and quality of life. Average age at surgery was 62.8 days. Serum bilirubin was normalized within three months in all patients. Six among the eleven long-term survivors had ascending cholangitis as one of the postoperative complications. The application of an intussusception anti-reflux valve did not show any statistical significance in long-term survival. Most of long-term survivors appeared to enjoy good quality of life. Kasai operation might not be the definitive treatment for biliary atresia; however, Kasai operation made it possible to achieve long-term survival for patients with biliary atresia when the patients were detected and treated as early as possible.
The aim of this study is to analyze the outcomes of the esophageal atresia with tracheoesophageal fistula over the last 2 decades. The records of 51 patients born between 1987 and 2006 were reviewed. Twenty-seven patients were male. Mean values of the age, gestational age and birth weight were 2.9 days, 296 days and 2.7kg, respectively. All patients had Gross type C anomalies. Thirty-one patients (60.7 %) had one or more associated congenital anomalies and the most common anomaly was cardiac malformation. In 48 cases, primary anastomosis was done and staged operation was done in one case. Circular myotomies in the proximal esophagus were performed in 9 cases. Postoperative complication developed in 26 cases (54 %): pulmonary complication in 12 cases, anastomotic leakage in 10 and anastomotic stricture in 10, recurrent trachoesophageal fistula in one and tracheomalasia in 2 cases. Reoperation was carried out in 2 patients with anastomotic leaks, the remaining leaks were managed non operatively. Three of the strictures were reoperated upon and the others were successfully managed by balloon dilatations. Overall mortality rate was 15.6 %. Mortality rate of the second 10 years (8 %) period decreased significantly compared to that of the first 10 years (23 %) period.
Citations

A vitelline duct (VD) anomaly is a relatively common congenital abnormality of the umbilical area. The anomalies include patent vitelline duct (PVD), cyst, fistula or sinus. The incidence is approximately 2% of the populations, but development of symptoms is rare. Recently, we experienced two cases; PVD accompanied by a smallomphalocele and intestinal volvulus due to mesenteric band between Meckel's diverticulum and the mesentery. Thereafter,we evaluated the data of vitelline duct anomalies for 27 years. From 1980 to 2006, 18 cases of VD anomalies were reviewed based on the hospital records retrospectively. There were 15 boys and 3 girls and age ranged from 2 days to 15 years. Among the 18 cases, 15 cases were symptomatic and consisted of Meckel's diverticulum (10 cases), PVD (4 cases) and umbilical polyp (1 case). Three asymptomatic cases of Meckel's diverticulum were found incidentally were and were observed without resection. Ten cases of Meckel's diverticulum were presented with intestinal bleedings (4 cases), intestinal obstructions (5 cases) and perforation (1 case). Wedge resections and segmental resections of ileum were performed in 8 patients and 2 patients, respectively. Postoperative complications were adhesive ileus (1 case) and wound seroma (1 case). Small omphaloceles were accompanied in two of 4 PVD patients. There was 1 small omphalocele case which was accompanied by a prolapse of ileum. In summary, VD anomalies were more common in male and more than half of them were found in patients less than 1 year of age. PVD was diagnosed most frequently in neonates. Meckel's diverticulum presented with intestinal obstruction more frequently than bleeding.
Citations

Tapering enteroplasty was first described by Thomas in 1969 as one method of intestinal anastomosis. The advantages of tapering enteroplasty in the intestinal atresia are: First, it makes end-to-end anastomosis possible between the atretic bowel ends with considerable differences in diameters. Second, it promotes the recover of the postoperative bowel function. Third, it prevents the possibility of the short bowel syndrome by eliminating the need of resecting the dilated bowel. A total of 22 patients with intestinal atresia who underwent tapering enteroplasty from January 1988 to December 2005 at our institute were reviewed. In 3 of 22 cases, tapering enteroplasty was the 2nd operation after an initial end-to-oblique anastomosis. We reviewed the following items: age, sex, type and location of intestinal atresia, initial feeding and total enteral feeding start day, the length of hospital stay and complications. The average age of the patients was 7 days. Male to female ratio was 1 to 1.2 (10 cases: 12 cases). We performed the tapering enteroplasty on all types and locations of the intestinal atresia from the duodenum to the colon: type I (n=3), type II (n=4), type IIIA (n=7), type IIIB (n=5), type IIIB and IV (n=1), type IV (n=1) and type C (duodenum) and type IIIB and IV (jejunum). On the average, the oral feeds were started on the postoperative 8.8th day, and full caloric intake via the enteric route was achieved on postoperative 13.3th day. The average length of hospital stay was 19.6 days. There were 1 case (4.5 %) of anastomotic complication and 2 cases (9 %) of adhesive ileus among 22 patients. The tapering enteroplasty on all types of intestinal atresia is a usefull operative method when there are considerable diameter differences between the atretic bowel ends.
Citations

Hereditary pancreatitis (HP) appears as an autosomal dominant trait. If the patient has (1) more than 2 affected relatives in different generations and (2) no known etiological factors such as alcohol or gallstones, or has R122H or N29I mutation in the cationic trypsinogen (CT) gene, the diagnosis of HP can be applied. Risk of pancreatic cancer is estimated to be 53-fold higher than in a general population after the age of 50 years. We report a kindredof HP, involving three of its family together; two siblings (14 years old, 13 years old) and cousin (26 years old). The patient had complicating chronic pancreatitis and pancreatic stone, and was treated with amodified Puestow-Gillesby procedure. Her sisters showed chronic pancreatitis. Her cousin underwent a drainage procedure of the pancreatic duct for chronic pancreatitis during the high school period. All the three members showed the R122H mutation of the CT gene.
Citations

Biliary atresia (BA) with extrahepatic biliary cysts (EHBC) is a rare disease. It has been generally recognized as type I (correctable with cystic dilatation), which means a good prognosis. From a total of 73 patients with BA who underwent operation from September 1988 to September 2003 at our institute, 7 (9.6 %) cases of type III BA with EHBC (uncorrectable with cystic dilatation) are reviewed. Clinical findings, laboratory data, radiologic findings, treatment methods and outcomes were reviewed. Female was more prevalent (male to female ratio; 2:5). All cases were type III with EHBC according to the intraoperative cholangiography, and underwent Kasai's portoenterostomy. The mean age was 57 days at operation. Three patients(42.9 %) are long term survivors. Further evaluation is needed to determine the correlation between prognostic factors and outcome for.
Appendectomy is the most common emergency surgical operation in children. The laparoscopic treatment of pediatric appendicitis is controversial, particularly in complicated cases. The purpose of this study is to evaluate laparoscopic appendectomy (LA) and open appendectomy (OA) for simple and perforated appendicitis (SA, PA) in children. A total of 188 patients, operated from January 1992 to September 2003, were reviewed. Ninety-one patients underwent OA (65 SA and 26 PA) and 97 had LA ( 67 SA, 30 PA). There was one conversion of LA to OA in PA. Operative time for LA was longer for OA in PA (55.8 vs. 45.7 min; p=0.0467). Recovery of bowel movement, diet starting time, length of hospital stay for LA were significantly shorter than those for OA. Postoperative complication rate was not different between LA and OA in each group. Laparoscopic appendectomy is a safe and effective method for both simple and perforated appendicitis.
Citations

Diagnosis of acute appendicitis in children is sometimes difficult. The aim of this study is to validate a clinical scoring system and ultrasonography for the early diagnosis and treatment of appendicitis in childhood. This is a prospective study on 59 children admitted with abdominal pain at St. Mary's Hospital, the Catholic University of Korea from July 2002 to August 2003. We applied Madan Samuel's Pediatric Appendicitis Score (PAS) based on preoperative history, physical examination, laboratory finding and ultrasonography. This study was designed as follows: patients with score 5 or less were observed regardless of the positive ultrasonographic finding, patients with score 6 and 7 were decided according to the ultrasonogram and patients above score 8 were operated in spite of negative ultrasonographic finding. The patients were divided into two groups, appendicitis (group A) and non-appendicitis groups (group B). Group A consisted of 36 cases and Group B, 23 cases. Mean score of group A was 8.75 and group B was 6.13 (p<0.001). Comparing the diagnostic methods in acute appendicitis by surveying sensitivity, specificity, positive predictive value, negative predictive value, and accuracy, PAS gave 1.0000, 0.3043, 0.6923, 1.0000, and 0.7288, and ultrasonography gave 0.7778, 0.9130, 0.9333, 0.7241, and 0.8300 while the combined test gave 1.0000, 0.8696, 0.9231, 1.0000, and 0.9490, respectively. Negative laparotomy rate was 3 %. In conclusion, the combination of PAS and ultrasonography is a more accurate diagnostic tool than either PAS or ultrasonography.
Citations

A newborn male baby was transferred to our hospital with a left inguinal mass. The mass was huge measuring 10 x 10 cm, engorged, and dark-blue colored as a result of internal hemorrhage. Unstable vital signs were combined with DIC and acute renal failure. Emergency operation was performed because of the suspicion of bowel perforation. The peritoneal cavity was full of ascitis and the distal jejunum had a 0.5 cm perforation. Segmental resection of the jejunum and incisional biopsy of the inguinal mass were performed. On pelvic and thigh MRI, the mass protruded into pelvic cavity and encircled large vessels and nerves of the thigh. Pathologic diagnosis was congenital infantile fibrosarcoma. Fifteen days after operation, primary tumor excision was undertaken. The second look operation, performed after 6 times VAC chemotherapy, revealed no remained malignant cell on microscopic section. The baby has been followed closely for the last eight months.
Diffuse cavernous hemangioma of the rectosigmoid is a rare lesion usually presented in children and young adult, often with life threatening hemorrhage. The clinical diagnosis is difficult and often delayed because of lack of awareness of the clinical features. We report a case of diffuse cavernous hemangioma of the rectosigmoid in a 12-year-old boy who had undergone suture ligation under the impression of hemorrhoid at his age 3. Sphincter-saving coloanal pull through procedure were applied as the surgical treatment. Sclerotherapy was needed with recurrent rectal bleeding 6 months after the pull through operation. The patient is well at 12 months follow-up.
When jaundice persists for more than 14 days postnatally, the early diagnosis of surgical jaundice is important for the prognosis in extrahepatic biliary atresia after draining procedure. The role of diagnostic laparoscopy to differenctiate medical causes of jaundice from biliary atresia is evaluated in this report. Four patients with prolonged jaundice have been included in this study. When the gallbladder was not visualized we proceeded to laparotomy. In patients with enlarged gallbladder visualized at laparoscopy, laparoscopic guided cholangiogram was performed, and laparoscopic liver biopsy was done for those who had a patent biliary tree. Two patients had small atretic gallbladder and underwent a Kasai hepato-portoenterostomy. One patients showed a patent gallbladder and common bile duct with atresia of the common hepatic and intrahepatic ducts, and they underwent a Kasai hepatic-portoenterostomy. One patient showed an enlarged gallbladder and laparoscopic-guided cholangiogram were normal. Laparoscopic liver biopsy was performed. There were no complications. Laparoscopy wth laparoscopic-guided cholangiogram may be a valuable method in accurate and earlier diagnosis in an infant with prolonged jaundice.
Mesenteric and omental cysts are rare intra-abdominal lesions in childhood, and may present various clinical features such as an asymptomatic mass or an acute abdomen. Therefore, these entities are frequently misdiagnosed preoperatively or are found only incidentally at operation for other conditions. We analyzed our experiences of 19 cases in a 19 year period from 1981 to 1999, at College of Medicine, Catholic University of Korea. There were 12 boys and 7 girls with a mean age of 4.8 years (range, 3 days to 15 years). Common presenting symptoms were abdominal pain (47%), abdominal distension (31%), abdominal mass (24%), vomiting (15%) and fever (10%). Ultrasonography was the most preferred method of diagnosis. Other diagnostic modalities include CT, MRI, and abdominal ascites tapping in selected patients. Location of the mesenteric cysts was small bowel mesentery in nine, the right mesocolon and retroperitoneum in one, the left mesocolon in one, and the jejunum, sigmoid-colon mesentery in one. Most of the patients underwent cyst excision, but six patients required concomitant bowel resection for complete removal of the lesions, and two patients underwent unroofing and simple aspiration respectively. There was one mortality case due to sepsis.
Citations

Childhood intussusception is usually idiopathic, and pathological lesions as the leading point are found in limited cases. Sixteen operative cases with leadpoints among 2,889 cases of childhood intussusecption treated at the surgical departments of the affiliated hospitals of Catholic University over 19 years are reviewed. The approximate incidence of pathological lesions as the leading point was 0.6%. The male to female ratio was 2:1. The mean age was 3.5 years. There was not an age preponderance. The symptoms were vomiting (63%), abdominal pain (38%), irritability (38%), bloody stools (25%), fever (25%) and abdominal mass (6%). The average duration of the symptoms was 2.4 days (1-10days). The most common lesion was Meckel's diverticulum, followed by malignant lymphomas, polyps, ectopic pancreas, and cecal duplication. An ileocolic type was most frequent, followed by ileoileocolic and ileoileal. Segmental resection or wedge resection of the ileum was done in 10 cases, ileocecectomy in 3, and right hemicolectomy in 3. Surgical reduction was done only in an ectopic pancreas, with no later recurrence. The average hospital stay was 10 days. Postoperative adhesive ileus occurred in two cases, and in one of them adhesiolysis was performed. One case of malignant lymphoma died at 28 days after surgery due to chemotherapy related complication.
Citations


