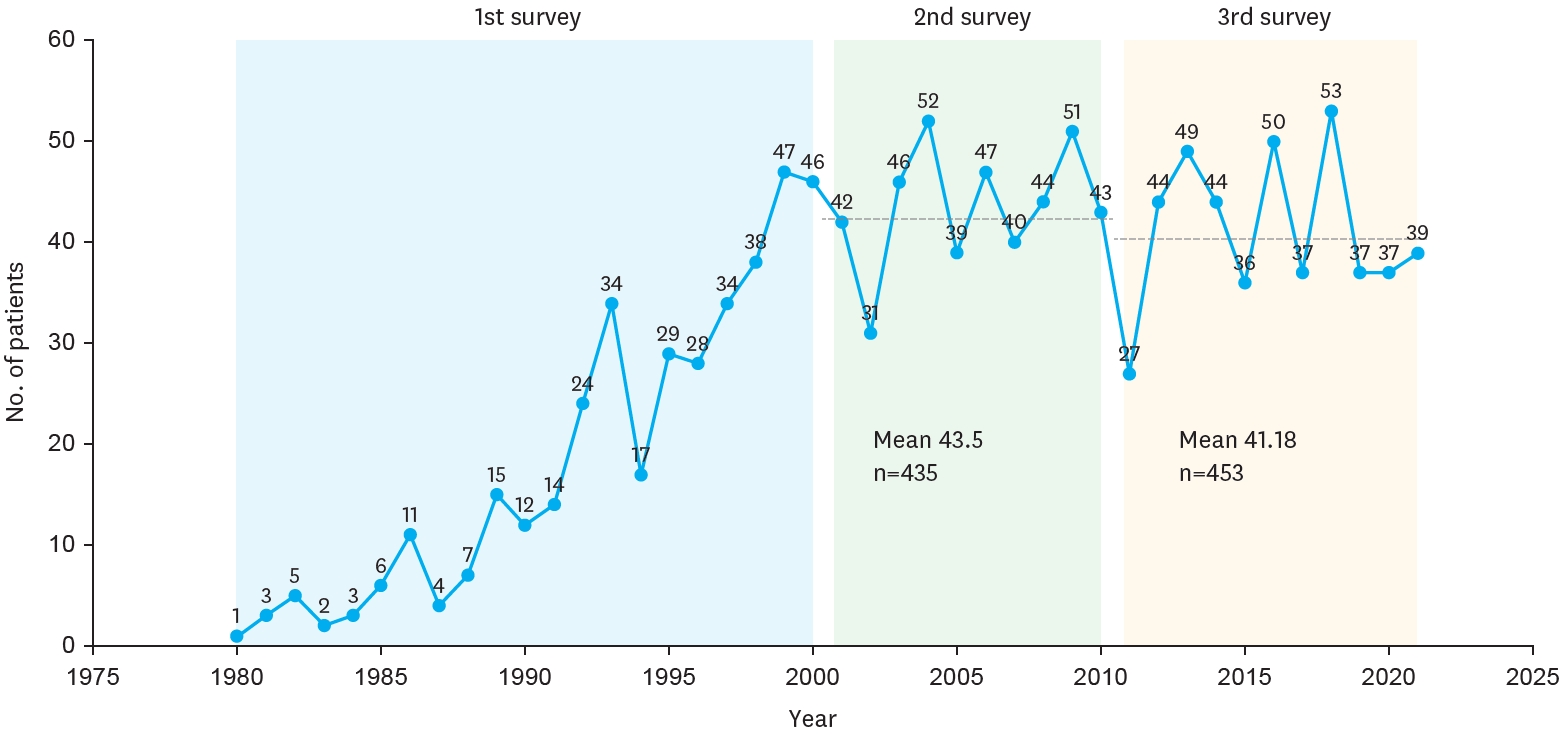
Branchial cleft anomalies are the second most common head and neck congenital lesions seen in children. Amongst the branchial cleft malformations, second cleft lesions account for 95 % of the branchial anomalies. This article analyzes all the cases of second branchial cleft anomalies operated on at Seoul National University Hospital from September 1995 to February 2011. We analyzed sex, age, symptom and sign, accompanied anomaly, diagnosis, treatment, pathologic report and outcome via retrospective review of medical records. In this series, we had 61 patients (27 female and 34 male). The mean age at the time of operation was 38 months. 31 lesions were on the right, 20 were on the left and 10 were bilateral. The most frequent chief complaints at presentation were non-tender mass and cervical opening without any discharge. According to anatomic type, 29 patients had branchial cleft sinuses, 14 had cysts, 14 had fistulas and 4 had skin tags. Complete excision was attempted if possible and antibiotics challenged when infection was suspected. Complete excision was achieved in 96.7 % of cases. Incision and drainage was done in 2 cases due to severe inflammation, and both recurred. Postoperative complications included wound infection in 2 cases. Microscopic examonation revealed squamous epithelium in 90.2 % and squamous metaplasia in one case in the branchial cleft cyst wall. In summary, second branchial anomaly is found more frequently on right side of neck. Fistulas are diagnosed earlier than cystic forms. Most cases could be diagnosed by physical examination. The definitive treatment is complete excision and sufficient antibiotics coverage for cases with inflammation. After drainage of infected lesions, follow up excision after 1 year might be beneficial for preventing recurrence.
Unreduced small bowel intussusception requires operative treatment although the rate of spontaneous reduction is 60 to 70%. The aim of this study is to compare clinical characteristics and outcome between spontaneous reduction and operation group and to analyze factors related to decisions to treat small bowel intussusceptions. The records of 25 patients with small bowel intussusceptions treated in Seoul National University Children's Hospital from January 1999 to August 2009 were reviewed respectively. Spontaneous reduction group (n=12, 48%) had signs and symptoms of vomiting, abdominal pain, currant jelly stool, abdominal distension, fever, increased CRP but no rebound tenderness. One of them had been diagnosed with Henoch-Schonlein purpura and no one displayed pathologic leading point by image study. Operation group (n=13, 52%) consisted of patients who had primary surgery. Their signs and symptoms were similar to spontaneous reduction group. Seven of them had underlying diseases such as Crohn' disease, ALL, Lymphoma, Peutz-Jeghers syndrome (n=3), post-transplanted state of liver and 2 of them displayed Peutz-Jeghers polyp and Meckel's diverticulum as pathologic leading point by preoperative ultrasonography. Mean relieve interval (interval between onset of symptoms and reduction/operation) was 1.78 days in spontaneous reduction group and 2.25 days in operation group (p=0.341). Seven of operation group had manual reduction and 6 out of 7 received segmental resection of the small bowel. No one of them underwent manual reduction and all of them underwent segmental resection were found to have pathologic leading points [Peutz-Jeghers polyp (n=3), Meckel's diverticulum (n=2), lymphoma (n=1)] during operation. In conclusion, 48% of small bowel intussusceptions resolved spontaneously. Patients' symptoms and relieve intervals were not related to the operative decisions. We therefore recommend significant factors for determining treatment plan such as change of clinical symptoms, underlying disease or pathologic leading point by imaging.
Air reduction is a safe, effective, and fast initial treatment for pediatric intussusception. There is low dose radiation exposure. Factors affecting outcomes of air reduction were analyzed by reviewing the clinical features and results of treatment. A total of 399 out of 485 patients with pediatric intussusceptions were treated at the Seoul National University Children's Hospital from 1996 to 2009. All of the patients received air reduction as the first line of treatment. Clinical features such as gender, age, seasonal variation, symptoms, signs, types, pathologic leading point, and treatment results including success rate, complication, recurrence, NPO time, and duration of hospitalization were reviewed. The Pearson chi-square, student T-, and logistic regression tests were used for statistical analysis. P-value less than 0.05 was considered to be statistically significant. The prevalent clinical features were: male (65.4%), under one-year of age (40.3%), ileocolic type (71.9%), abdominal pain (85.4%), and accompanying mesentery lymph node enlargement (2.2%). The overall success rate for air reduction was 78.4% (313 of 399 patients), and the perforation rate during reduction was 1.5%. There were 23 recurrent cases over 21.6 months. All were successfully treated with re-do air reduction. Reduction failures had longer overall NPO times (27.067hrs vs. 43.0588hrs; p=0.000) and hospitalization durations (1.738d vs. 6.975d; p=0.000) compared to the successful cases. The factors affecting success rates were fever (p=0.002), abdominal distension (p=0.000), lethargy (p=0.000) and symptom duration (p=0.000) on univariate analysis. Failure rates were higher in patients with symptom durations greater than 24 hours (p=0.023), and lethargy (p=0.003) on multivariate analysis. Air reduction showed high success rates and excellent treatment outcomes as the initial treatment for pediatric intussusception in this study. Symptom duration and lethargy were significantly associated with reduced success rates.
Citations

Condyloma acuminatum is an uncommon disease but there is an increased incidence reported in recent years in prepubertal children. Anal and perianal condyloma accuminatum in children may suggest sexual abuse and treatment should include the thorough social evaluation as well as medical treatment. A 25 month old girl presented with multiple sessile nodules around her anal and perianal area, Biopsy confirmed the diagnosis of condyloma accuminatum. There was no definite evidence of sexual abuse, but her father had condyloma accuminatum involving his penis. The patient's lesions were excised totally. At three week follow up there was no anal stricture but there were newly developed small lesions around perianal area. Imiquimod onit was applied for 2 weeks and the recurred lesion disappeared completely. At postoperative 5 month, the operative area was fully epithelialized without recurrence.
Citations

Pancreaticoduodenectomy is the treatment of choice for adult periampullary lesions. However there has been no studies on the clinical outcomes of pancreaticoduodenectomy in children. To evaluate the clinical outcomes, records of 13 patients who underwent pancreaticoduodenectomy, from 1989 to 2009, at Seoul National University Children's Hospital were reviewed. Mean follow up period was 83 (2-204) months, the male to female ratio was 1:3.3, and the mean age was 11 (2-14) years. Ten patients underwent PPPD and 3 patients had Whipple's operation. The postoperative diagnosis included solid pseudopapillary tumor (9), cavernous hemangioma (1), pseudocyst (1), benign cyst (1), pancreatic disruption (1). Two patients developed postoperative adhesive ileus and among them one patient required operative intervention. Four patients required pancreatin supplementation due to steatorrhea and other gastrointestinal symptoms. There were no postoperative mortality during the follow up period and no evidence of recurrence in SPT patients. This study demonstrates that the pancreaticoduodenectomy procedure in children is not only feasible but also safe, with no mortality and an acceptable complication rate.
Congenital thoracic malformations such as intra- and extra-pulmonary sequestration, cystic adenomatoid malformation, congenital pulmonary airway malformation, malinosculation, bronchogenic cyst, reduplication cyst, and foregut cyst are frequently detected on routine prenatal ultrasound. There are some controversies about treatment for postnatally persistent pulmonary sequestration. Some authors recommend expectant long term follow up but most authors advocate elective surgical excision because of complication such as respiratory distress, infection, intrathoracic bleeding, haemoptysis, cardiac failure, and potential risk of malignancy. We experienced 2 cases of prenatally diagnosed extrapulmonary sequestration which were located in the subdiaphragmatic retroperitoneum. Resections were performed at 2 months and 4 months of age using intraabdominal approach. There were no complications. In conclusion, if the prenatally diagnosed extrapulmonary sequestration remained postnatally, early operation might reduce morbidity related to extrapulmonary sequestration and parental anxiety without any postoperative complication.
Colorectal cancer is extremely rare in children. Unlike adult colorectal cancer, the overall prognosis of colorectal cancer in children is poor. Delayed diagnosis, advanced stages of the disease at presentation, and mucinous type of histology are the major determinants of poor outcome in childhood. A 13-year-old boy with abdominal pain visited our hospital. Physical examination andabdominal ultrasonography identified acute appendicitis with perforation. He underwent appendectomy and then the pathologic findings revealed mucinous adenocarcinoma. The cancer was located at the transverse colon and had metastases on peritoneal wall at 2nd laparotomy. Extended right hemicolectomy was performed. He underwent palliative chemotherapy. After 4 months later, hepatic metastasis and aggravated peritoneal seedings developed. He died of renal failure and pneumonia 13 months after operation. We need to have a high index of suspicion for the possibility of a malignant colorectal tumor in any childhood case with nonspecific signs and symptoms.
Inflammatory myofibroblastic tumor (IMT) is a rare reactive lesion characterized by the feature of myofibroblasts and a mixed inflammatory infiltrate that rarely undergoes malignant transformation. Extrapulmonary IMTs in children have been described involving the mesentery, omentum, retroperitoneum, abdominal soft tissues, liver, bladder, mediastinum, head and neck, extremity, appendix, and kidney. Medical records of children treated with abdominal IMT between 1985 and 2005 were reviewed retrospectively. Seven children were treated for IMT with the mean age of 3y 2m (range, 1y 1m to 14y). Tumors were located in transverse mesocolon (n=2), omentum (n=1), porta hepatis (n=2), complex site (antrum, duodenum, common bile duct, porta hepatis) (n=2). The symptoms included abdominal mass, fever, jaundice, abdominal pain and anemia. The masses were excised totally in transverse mesocolon, omentum IMT and there is no evidence of recurrence (follow-up periods: 6y 8m, 8y 9m, 4y 10m). In porta hepatis IMT, liver transplantations were performed and there is no evidence of recurrence (follow period: 6y 8m, 8y 7m). In one case of complex site IMT, partial excision of mass was performed and he still survived with no change of the residual tumor during follow-up period. The other one of complex site IMT denied further treatment after the biopsy. In conclusion, complete surgical excision including liver transplantation and close follow-up are mandatory for the abdominal IMT in child.
Citations

Thyroid nodules are less common in children than in adults and their management is still controversial. The clinical presentations, operations, complications, histopathologic findings, and postoperative progressions of 34 pediatric patients that underwent thyroidectomy for palpable thyroid nodule at the Department of Surgery, Seoul National University Children Hospital between 1986 and 2003 were studied retrospectively by reviewing medical records and telephone interviews. The mean age of the patients was 11.8 years old. There were 23 females (67.6 %) and 11 males (32.4 %). Surgical indications were clinical need of histological confirmation (n=15), unresponsiveness to thyroxin replacement therapy (n=10), suggestion of the carcinoma on fine needle aspiration cytology (n=5), cosmetic purpose-a huge benign nodule (n=2), completion thyroidectomy for medullary thyroid carcinoma (n=1), and prophylactic thyroidectomy in a MENIIpatient (n=1). Unilateral Lobectomy was performed in 20 patients (57.1 %), subtotal thyroidectomy in 8 (22.9 %), total thyroidectomy in 5 (14.7 %), and completion thyroidectomy in 1 (2.9 %). Lymph node dissection was performed in 9 cases. Benign tumor was found in 23 patients (67.6 %), adenomatous goiter (n=18) and follicular adenoma (n=5). Malignant tumor was found in 11 children (32.4 %), 9 papillary carcinomas (26.5 %), and 2 medullary carcinomas (5.9 %). Of the 9 papillary carcinomas, 7 cases (77.8 %) had lymph node metastasis. No lymph node metastasis was found in 2 medullary carcinomas. Complications developed in 5 cases - transient hypocalcaemia (n=2), and temporary hoarseness (n=3). There was no mortality. Median follow-up period was 7.4 years (0.5-18 years). One patient showed recurrence in cervical lymph nodes 10 years after surgery and modified radical neck dissection was performed. Because of the high incidence of malignancy and advanced stage at initial presentation, more meticulous diagnostic work up is necessary for children with thyroid nodule, and more radical surgical treatment should be performed when malignant nodule is suggested.
Citations

A 3-year-old girl with a primitive neuroectodermal tumor (PNET) and a 6-year-old girl with acute lymphoid leukemia were referred to us because of problems with their implantable central venous ports (Port-A-Cath®). On physical examination, the ports were upside-down, so a needle could notbe inserted through the membrane of the port. Right lateral side view of the chest radiogram confirmed port inversion in both cases. At operation, the ports were inverted and the transfixing sutures were totally absorbed. The ports were rotated 180 ° and anchoring sutures placed.
Citations

Ulcerative colitis, one of the inflammatory bowel disease, is primarily managed medically with combinations of 5-ASA and steroids. However, this chronic disease requires surgical management if symptoms persist or complications develop despite medical management. The clinical course, the indications and outcome for surgical management of pediatric ulcerative colitis patients were studied from medical records retrospectively. Twenty-one patients under the age of 15 who were endoscopically diagnosed with ulcerative colitis at the Seoul National University Children's Hospital between January, 1988 and January, 2003 were subjected to the study. Mean follow up period was 3 years and 10 months. The mean age was 10.3 years old. All patients received medical management primarily after diagnosis and 8 patients (38%) eventually required surgical management. Of 13 patients who received medical management only, 7 patients (53%) showed remission, 4 patients are still on medical management, and 2 patients expired due to congenital immune deficiency and hepatic failure owing to sclerosing cholangitis respectively. In 8 patients who received surgical management, 1 patient underwent surgery due to sigmoid colon perforation and 7 patients due to intractability of medical management. The perforated case received colon segmental resection and the other 7 patients recieved total protocolectomy with ileal pouch-anal anastomosis. One patient expired postoperatively due to pneumonia and sepsis. One patient is still on medical management because of mild persistent hematochezia after surgery. The other operated patients are showing good prognosis without any management. Pediatric ulcerative colitis patients can be surgically managed if the patient is intractable to medical management or if complications such as perforation is present. Total protocolectomy & ileal pouch-anal anastomosis is thought to be the adequate surgical method.
The purpose of this study is to review the operative management and outcome of operation for Crohn's disease. The medical records of 17 patients who underwent operations due to Crohn's disease at Seoul National University Children's Hospital from January of 1988 to June of 2005 were reviewed and retrospective study was carried out. The male-to-female ratio was 1.8: 1. The median age at the onset of symptom and the time of diagnosis was 9 years 6 months and 11 years 6 months respectively. The median interval time from diagnosis to operation was 2 years and 1 month (0 month~8 years). Ileocolic or ileocecal region was the most common site of involvement. The indications of operation were intractable symptoms (8 cases) and obstruction or stricture (7 cases). The median postoperative hospitalized days were 14.4 days (8~35 days). Five patients (29%) experienced postoperative complications. Symptom free state or symptom relief was observed in 11 cases after surgery and 6 cases had wax and wane course of aggravation and improvement. In pediatric Crohn's disease patients who present with intractable symptoms despite medical treatment or develop surgical complications, symptom free state or symptom relief can be achieved by minimal resection of involved lesion.
Citations

Primary liver tumors are uncommon in childhood, with a relative frequency of 3% of childhood tumors. Seventy three cases of pediatric primary liver tumors which were operated on at single institution between 1986 and 2002 were reviewed. There were 37 cases of hepatoblastoma, 11 hepatocellular carcinomas, 6 undifferentiated (embryonal) sarcomas, and 1 mixed germ-cell tumor in malignancies. Benign tumors constitute only 24.6% of liver tumors, including 7 hemangioendotheliomas, 5 mesenchymal hamartomas, 3 congenital cysts, and one each with focal nodular hyperplasia and hemangioma. The common presenting clinical features were abdominal mass or abdominal distension. Anatomical hepatic resections were carried out in 38 cases, and non anatomical resections in 34 cases. One patient died of a direct result of hepatic resection(1.4%), and complication rate was 16.4%.
Choledochal cysts have been associated with complications such as cholangitis, pancreatitis, and malignancy of the biliary tract. Recently, the incidence of choledochal cyst in neonate and young infant is increasing due to advances in diagnostic imaging. The aim of this study is to investigate the rationale of excision of choledochal cyst during the neonatal period. The clinical outcome and correlation between age at surgery and the degree of liver fibrosis were reviewed retrospectively. A total of 198 patients with choledochal cyst who were managed surgically between January 1985 and December 2000 at the Department of Surgery, Seoul National University Children's Hospital were included in this study. The overall outcome and the outcome of patients who were managed surgically during the neonatal period were compared. Correlation between age and the degree of liver fibrosis was evaluated by chi-square test and Pearson exact test. The mean age of the patients was 2 years 7 months (ranged from 5 days to 15 years). Mean postoperative follow-up period was 7 years 1 month (7 months to 20 years). The results are as follows. Twelve patients (6%) had postoperative complications, cholangitis (7), bleeding (4) and ileus (1). Eleven patients operated during the neonatal period had no postoperative complications. The positive correlation between age group and degree of liver fibrosis was statistically significant (chi-square: p=0.0165, Pearson exact test: p=0.019). The results support the rationale that excision of choledochal cyst can be performed safely without increasing morbidity in neonates.
With the development of fetal ultrasonography, detection of fetal ovarian cysts has been increased. Although ovarian cyst formation during the perinatal period is a self limiting process, there is still considerable controversy regarding the best treatment of the fetal ovarian cyst. The purpose of this study is to evaluate the natural history of fetal ovarian cysts and to analyze the result of treatment. From 1995 to 2004, 31 consecutive fetuses with ovarian cysts were followed by ultrasonography during the perinatal period. The fetal ovarian cyst was diagnosed by prenatal ultrasonography between 25weeks and 38 weeks and the mean size of the cysts was 5cm (ranged from 2 to 8cm). At birth, 3 cysts disappeared. In 2 cases, the diagnoses were changed to multicystic kidney disease and intestinal duplication. During following up of 26 cysts, 15 cysts have resolved completely. Seven cysts required oophorectomy because of cyst torsion (n=3), differentiation of tumorous condition (n=2), increased size of cyst (n=1), and large size (8cm) of cyst at birth (n=1). Fetal ovarian cyst should primarily be observed, and only in the limited cases, surgical treatment would be required for the risk of complications such as torsion and differentiation from benign to malignant pathology.
The history of esophageal replacement in infants or children is the history of development of various kinds of alternative conduits such as stomach, colon, and small bowel. The gastric tube has been the most widely used conduit. From January 1988 to May 2003, 23 esophageal replacements with gastric tube were performed at the Department of Pediatric Surgery, Seoul National University Childrens Hospital. Statistical analysis was performed using Windows SPSS11.0 Pearson exact test. There were Gross type A(n=10), type B(n=1), type C(n=11), type D(n=1). Ten patients who had long gap esophageal atresia (type A-8, type B-1, type C-1) and 13 patients (type A 2, type C-10, type D-1) who had stenosis, leakage, recurred tracheoesophageal fistula, and esophagocutaneous fistula after previous corrective operations, had esophageal replacement with gastric tube. Mean follow-up periods were 4 year 2 months (7 months-15 year 1 month). There were postoperative complications including GERD in 16 (69.6 %), leakages in 7 (30.4 %), diverticulum at anastomosis in 2 (8.7 %), anastomosis site stenosis in 4 (17.3 %), and distal stenosis of the gastric tube in 1 (4.3 %). There was no statistical significance between operation types and postoperative leakage and gastroesophageal reflux. In conclusion, esophageal replacement with gastric tube may be a useful surgical option in esophageal atresia with long gap and esophageal atresia complicated by previous corrective operation.
As prenatal ultrasonography becomes popular, the number of prenatal diagnosis of congenital surgical diseases is also increasing. To evaluate the impact of antenatal ultrasonography on outcome the mortality rate in neonatal surgical emergencies was studied. The authors retrospectively reviewed 281 patients (congenital diaphragmatic hernia: 44, tracheoesophageal fistula: 78, intestinal atresia: 98, omphalocele: 28 and gastroschisis: 33 who had been managed at Seoul National University Childrens Hospital, from January 1991 to December 2000. The patients were divided into two groups; group A (1991 to 1995; 139 patients) and group B (1996 to 2000; 142 patients). These two groups were subdivided into prenatally diagnosed subgroup and postnatally diagnosed subgroup. We analyzed the changes of prenatal diagnosis rate, total mortality rate, and mortality rate of subgroups. Prenatal diagnosis rate was increased significantly in group B (Group A: 24.5 % and Group B: 45.1 %). Total mortality rate of group A was 21.6 %, and that of group B was 10.6 %, showing a significant decrease in group B. However, in both group A and B, when compared antenatally diagnosed subgroup with postnatally diagnosed subgroup, the mortality rate was lower in postnatally diagnosed subgroups but statistically not significant. The authors conclude that although prenatal diagnosis rate has been increased, prenatal diagnosis itself has not resulted in significant improvement in outcome.
A 12-year-old boy with severe periumbilical pain visited the emergency room. Physical examination, abdominal ultrasonography, colonoscopy and CT, identified a lesion of sigmoid colon. Endoscopic biopsy showed a signet ring cell carcinoma of the sigmoid colon. On explorative laparotomy, cancer invasions of the adjacent structures and metastases on peritoneal wall were noticed. We performed palliative loop-ileostomy. He underwent chemotherapy and radiotherapy for 3 months. The second case was a 16-year-old boy with abdominal pain and hematochezia, transferred to our hospital with the diagnosis of acute appendicitis with periappendiceal abscess. Although he underwent appendectomy, the abdominal pain persisted. Digital rectal examination revealed a lumen-obstructing fungating mass in the rectum. Endoscopic biopsy revealed a adenocarcinoma. Cancer invasion of the adjacent structures and metastases involving the mesentery of the small intestine were found at laparotomy. A palliative procedure, a Hartmann's operation and end-colostomy at the sigmoid colon were performed. The patient died 8 month later due to pneumonia and sepsis. Chemotherapy was not applied.
Visceral leishmaniasis is a life-threatening systemic infection caused by a protozoa of the genus leishmania and transmitted by sandfly. We report the first case of visceral leishmanaisis in Korea. The patient was a one-year-old girl admitted with the symptoms of fever, abdominal distension, pancytopenia, and purpura. She traveled to Argentina 5 months ago, and has had symptoms such as fever and pale appearance. Laboratory findings were: WBC, 12,680/mm3; Hg, 3.7g/dL; platelet, 100K; total bilirubin, 1.2mg/dL; AST/ALT, 48/10 U/L. CT scan and MRI showed hepato-splenomegaly. On laparotomy, excision of an accessory spleen and splenic hilar lymph nodes were performed. Many amastigotes were microscopically identified in histiocytes from the biopsy tissues. Sodium stibogluconate was administrated for 2 weeks, which did not relieve the symptoms. After administration of the additional Amphotericin B for 3 weeks, symptoms were improved.
Citations

A re-pull-through operation for Hirschsprung's disease is performed when the primary operation has failed because of the remnant or acquired aganglionosis, anastomotic stricture and/or fistula. The purpose of this study is to review our experience of the re-pull-through procedure for Hirschsprung's disease. From May 1978 to July 2003, 26 patients who underwent re-pull-through operations at the Department of Pediatric Surgery, Seoul National University Children's Hospital, were studied retrospectively by means of chart review as well as telephone interview. The mean age at primary operation and re-operation were 11months (2 months - 10 years) and 43 months (1 year - 23 years 3 months), respectively. Initial operation for Hirschsprung's disease was Duhamel's procedure in 17, Swenson's in 6 and Soave's 3. Causes of failure of primary operation were remains of secondary aganglionic segment (n=23), vascular arcade injury (n=1), rectoperineal fistula (n=2, due to mesenteric torsion and poor blood supply). Mean interval between the primary operation and the re-operation was 34 months (6 months-22 years). Reoperation methods were Soave's in 12, Duhamel's in 8, APSP (abdomino-posterosagittal pull-through procedure) in 5, and Swenson's in 1 case. In 2 cases of repeated rectoperineal fistula or rectourethral fistula, re-APSP were performed 3 times, respectively. A total of 29 re-pull-through operations were performed. Postoperative complications were wound infection (n=1), adhesive ileus (n=1), rectoperineal fistula (n=3), rectourethral fistula (n=2), and death due to pulmonary embolism (n=1). Mean follow up period of reoperation was 78 months (1 month-23years). In current state, 2 patients have an ileostomy because of repeated rectoperineal fistula and rectourethral fistula. Of the remaining 23 patients, 21(91 %) are totally continent with or without minimal soiling. Reoperation for Hirschsprung's disease was effective and safe for the patients complicated to the initial pull-through operation.
Citations

Inguinal hernia is a major surgical disease in pediatric surgery, occurring in 3.5% to 5% of all mature newborns and 9% to 11% of all premature babies. The
objective
of this study is to analyze the predisposing factors in association with recurrences of inguinal hernias in infants and children. In the period from January 1995 to September 2001, 1,575 infants and children who had primary inguinal hernias and recurrent inguinal hernias operated on at the Department of Pediatric Surgery at Seoul National University Hospital were evaluated retrospectively. We evaluated the data by medical records and by telephone interview. The sex, age, location of hernia, comorbidity, prematurity, incarceration, interval to operation after incarceration, postoperative complications were analyzed as predisposing factors in associated with hernia recurrence. Operative findings of recurrent inguinal hernia were reviewed. The data were statistically analyzed with Pearson Chi-Square test and Fisher-exact test. A total of eighteen (1.14%) out of 1,575 patients underwent an operation due to recurrent inguinal hernia. In 5 (27.8%) out of 18 recurred patients, institution of the primary herniorrhaphy was our hospital and in the other 13 (72.2%) was outside hospital. No impact on the development of recurrences was seen for sex, age, interval to operation after incarceration, and postoperative complications. The significant predisposing factors of recurrent inguinal hernias were left inguinal hernias (p=0.002), comorbidity (p=0.002), prematurity (p=0.006), incarceration (p=0.017) and technical error of first herniorrhaphy. We expect that knowledge for predisposing factors of recurrent inguinal hernias and experienced skill of pediatric surgeons will decrease recurrence rate in primary inguinal hernia.
The aim of this study was to evaluate the posterior sagittal anorectoplasty (PSARP) as a re-do operation in patients who failed initial repair of anorectal malformation. Nine patients (4 boys and 5 girls) who had previous failed surgery for anorectal malformation underwent secondary operations through posterior sagittal approach. The main reasons of surgery were constipation (n=3) and persistent anatomical derangement in spite of previous correction surgery (n=6). In addition to constipation, the former group (n=3) had various anatomical defects, and the latter group (n=6), of course, had constipation in some degrees. Patients ranged in age from 2 to 19 years (median 3 years) with only one over the age of 6 years. The primary procedures included PSARP (n=8) and anoplasty (n=1). The rectum was mobilized from surrounding structures through posterior sagittal approach and anatomical defects were corrected. The rectum underwent reconstruction, which involved relocation of the rectum and anus within the limits of the intact muscle complex. Patients underwent follow-up for periods ranging from 6 to 77 months (mean 37 months) after surgery. Anatomical corrections of all the defects were successfully fulfilled in 9 patients. All the patients were satisfied with the functional results after redo-PSARP compared with the preoperative defecatory function. This study suggests that (1) some of the patients with troublesome constipation may have anatomical defects, prominent or hidden, (2) surgeons should suspect the possibility of anatomical defect as the cause of incontinence and (3) preoperative thorough investigation to reveal the anatomical defects should be included in estimating patients with severe incontinence after previous surgery and planning the correction for failed previous surgery as well.

